Abstract
Background: Within the heterogeneity of schizophrenia, apathy constitutes an independent cluster of negative symptoms associated with poor outcomes. Attempts to identify an emotional deficit in patients who have schizophrenia with negative symptoms have yielded mixed results, and studies that focus on the relationship between apathy and emotional disorders are lacking.
Methods: We set out to remedy this shortcoming using a validated battery of film excerpts to induce positive and negative emotions in patients with chronic schizophrenia with (n = 20) or without (n = 20) apathy, and in controls (n = 20) comparable for age, sex and socioeconomic status. We assessed emotions using an innovative but validated technique to evaluate tonic and phasic electrodermal activity and subjective feelings using a standardized visual analogue scale.
Results: Using a qualitative measure of apathy, we did not find a specific decrease in tonic activity during the induction of positive emotions. However, we did observe that patients with apathy showed reduced tonic activity independent of valence (i.e., for both positive and negative emotions) compared with controls and patients without apathy. Moreover, the quantitative measure of apathy (Apathy Evaluation Scale) was the only significant factor, explaining 24% of the variance in tonic activity during induction of positive emotions after controlling for confounding factors.
Limitations: Electrodermal activity was the only physiologic measure we acquired. We induced several emotions sequentially that might have overlapped with each other, but we added an emotional “washout” period and randomized the order of each film excerpt to limit this possibility.
Conclusion: Taken together, these results suggest that apathy in schizophrenia could impair tonic activity during positive emotions. Treatments aimed at enhancing positive emotions may help alleviate apathy in schizophrenia.
Introduction
Schizophrenia induces emotional impairments, causing social dysfunction.1 Negative symptoms in schizophrenia are heterogeneous, but can be grouped into 2 independent clusters: apathy/avolition and diminished emotional expression.2 Apathy is defined as a lack of motivation that reduces the emotional, cognitive and behavioural components of goal-directed behaviours in daily life.3,4 It accounts for the largest proportion of poor functioning in daily life and overall outcomes in schizophrenia, independent of cognitive impairment5 and diminished emotional expression.6 People with schizophrenia and apathy show steeper reward devaluation in relation to physical effort than patients without apathy.7 However, emotional deficits in schizophrenia with apathy have been unexplored. This is unexpected, because motivation is a key component of emotional processing in contemporary models,8 and altered emotional processing has been highlighted in Parkinson disease with apathy,9,10 suggesting that apathy might impair emotional processes.
Previous investigations into subjective emotional experiences in schizophrenia have opted for laboratory-based eliciting of emotion, using a wide variety of stimuli (e.g., odours, food, emotional faces or pictures).11 Despite such methodological heterogeneity, most studies have found that patients with schizophrenia experienced positive emotions in a similar way to healthy controls.1,12 However, some results have suggested exacerbated negative emotional experiences in response to positive or neutral stimuli,13,14 or impaired neural response to positive stimuli in schizophrenia.15,16 One approach to explaining preserved hedonic capacity in schizophrenia separates goal-directed emotions into reward anticipation and intact positive emotions during reward reception.1,17 The results of previous studies support the hypothesis that apathy in schizophrenia and in healthy people with psychotic-like symptoms is associated with blunted striatal response during reward anticipation, but not during reward reception.18–20
Emotional processes include electrodermal activity (EDA) as a marker of emotional arousal.21 Few studies have explored the link between subjective emotional experiences and EDA during emotional induction in schizophrenia, and results have been mixed: studies found greater, equal or reduced EDA in response to emotional pictures.22–24 Electrodermal activity reflects autonomic nervous system activity and can be divided into tonic (slow variations) and phasic (rapid variations) activity.25 More specifically, tonic EDA activity refers to skin conductance level, and phasic activity corresponds to a skin conductance reaction (SCR) evoked by a stimulus.25 A recent review found that tonic and phasic activities can be increased during emotional episodes using various methods of emotion induction (film excerpts, music or pictures) and across all emotional categories (joy, fear, anger, surprise).21 Phasic activity is a rapid and event-related feature of EDA, but tonic activity is associated with anticipation of an outcome during conditional paradigms of long duration.26 Moreover, reduced tonic EDA has been related to apathy in a population with brain injuries.27
Because apathy has been related to the decreased ability to anticipate positive emotions in schizophrenia, and because anticipation of an outcome is associated with tonic EDA, our primary objective was to test for reduced tonic activity during the induction of positive emotions in patients with schizophrenia and apathy, compared to patients with schizophrenia without apathy and healthy controls. Our secondary objective was to examine whether quantitative apathy scores were associated with tonic activity during positive emotion when controlling for confounding factors in patients with schizophrenia.
To this end, we induced discrete positive and negative emotions using a validated battery of film excerpts28 and extracted tonic activity from EDA recordings in comparable groups of patients with schizophrenia with and without apathy, and in a control group.
Methods
Participants
We recruited 20 outpatients who had stable chronic schizophrenia (fewer than 3 positive items scored 4 or above on the Positive and Negative Syndrome Scale29 [PANSS] and no medication changes during the previous 2 months) and apathy (Scz-A), and 20 patients who had schizophrenia without apathy (Scz-NA), all from Rennes University Hospital in France. All participants were native French speakers. We recruited healthy controls using local advertising. Eight patients refused to participate in our study. We recruited participants to build 3 groups that were comparable in terms of age, socioeconomic status, sex, handedness and disease duration. We also recruited patients so that the chlorpromazine-equivalent dose was similar between both groups. All patients were ambulatory.
Schizophrenia had been diagnosed according to the French version of the Mini International Neuropsychiatric Inventory, 30 based on DSM-IV-TR criteria.31 Exclusion criteria included psychotic depression, severe extrapyramidal symptoms and low-order visual and auditory impairments. Patients were allocated to the Scz-A or Scz-NA group according to the diagnostic criteria for clinical apathy.6 Apathy was assessed quantitatively using the Apathy Evaluation Scale (AES).32 The clinical criteria and the AES have been validated in schizophrenia.4
All patients were being treated with medication at the time of testing. In the Scz-A group, 16 patients were receiving atypical antipsychotics and 4 were receiving both atypical and typical antipsychotics; 4 were receiving benzodiazepines. In the Scz-NA group, 19 patients were receiving atypical antipsychotics and 1 was receiving a typical antipsychotic; none were receiving benzodiazepines.
Twenty healthy controls received €50 for their participation and were not taking any medications. Patients did not receive monetary compensation, following French ethics recommendations.
Exclusion criteria for all participants were neurologic and systemic illness, previous head injury, severely impaired vision or auditory acuity, and mental retardation (Mattis Dementia Rating Scale33 score below 120). As well, any diagnosis of a mental disorder according to the Mini International Neuropsychiatric Inventory led to exclusion in the control group.
Written informed consent was obtained from each participant, and the study met the ethical standards of the Declaration of Helsinki. The study was approved by the local ethics committee (CPP Ouest II-Angers Number: 2012/16).
Psychopathological and neuropsychological assessment
We used the PANSS29 to assess the stability and severity of schizophrenia. We assessed overall negative symptoms using the Scale for the Assessment of Negative Symptoms (SANS)34 and depressive symptoms using the Calgary Depression Scale for Schizophrenia.35 We used the Abnormal Involuntary Movement Scale36 to assess extrapyramidal symptoms.
The executive function battery included phonemic and semantic fluency tests, an adapted version of the Stroop paradigm, the Trail Making Test (TMT) and the digit span and digit symbol coding subtests of the Wechsler Adult Intelligence Scale IV. See a study by our group37 for a complete description of the battery.
Emotion elicitation procedure
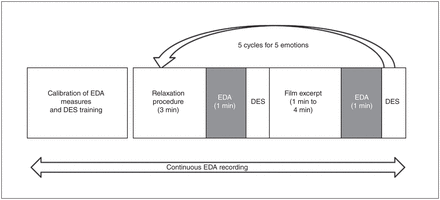
Film excerpts are effective, valid and powerful for eliciting intense and specific target emotions.38–40 We used a battery of 5 film excerpts, selected from a larger validated battery28 according to their likelihood to induce a specific subjective emotional experience: happiness, anger, fear, sadness or disgust. All excerpts were in French, lasted 1 to 4 minutes, and were displayed on a 22-inch colour screen. The film excerpts had been edited to produce the apex of emotional intensity as they ended (Philippot P., personal communication, Nov. 15, 2017). To capture the emotional peak and standardize excerpt length, we analyzed the EDA recordings for only the last minute of each excerpt. We randomized the order of presentation for each participant so that no one experienced them in the same order. Before each excerpt, participants went through a 3-minute relaxation procedure to “wash out” previous emotions. After the washout period, we captured EDA for 1 minute to obtain a baseline before eliciting the next emotion (Fig. 1).41
Procedure for emotional induction. First, we performed a calibration of EDA measures using a period of relaxation. Then, we ran 5 cycles using 5 different film excerpts that targeted 5 emotions in random order, with continuous recording of EDA. Each cycle began with a relaxation procedure (3 min), followed by acquisition of a baseline EDA value and a first subjective emotional rating using the DES. Then, a target emotion was induced using a film excerpt. We used the final minute of the film excerpt for EDA processing, and then a second subjective emotional rating (DES) was performed. DES = Differential Emotion Scale; EDA = electrodermal activity.
Assessment of subjective emotional experience
After each relaxation and presentation phase, participants reported the intensity of their emotional experiences on the Differential Emotions Scale,41 which consists of 10 visual analogue scales: 1) interested, concentrated, alert; 2) joyful, happy, amused; 3) sad, downhearted, blue; 4) angry, irritated, mad; 5) fearful, scared, afraid; 6) anxious, tense, nervous; 7) disgusted, turned off, repulsed; 8) disdainful, scornful, contemptuous; 9) surprised, amazed, astonished; 10) warmhearted, gleeful, elated. Each scale ranged from 0 (no subjective emotional experience at all) to 7.5 (very intense subjective emotional experience).
Assessment of EDA
We acquired EDA following the recommendations of the Society for Psychophysiological Research.42 Two surface bipolar finger electrodes (Model MLT 118F; ADIntruments) were placed on the pad of the left forefinger and middle finger, without isotonic paste to preserve the natural condition of the skin. We recorded EDA using an isolated amplifier (ML116 GSR Amp; ADInstruments) connected to a PowerLab/4SP system (ADInstruments) using constant-voltage excitation (22 mVrms at 75 Hz). The signal was recorded continuously using Labchart v7.4.1 software (ADInstruments) at a sampling rate of 10 Hz. The temperature of the room was constant (approximately 20°C). Before the emotion elicitation procedure, EDA was recorded during a training session with the relaxation procedure to calibrate the EDA recording and train the participant on filling out the DES. Participants were excluded if the EDA recording did not meet the criteria for data quality (many artifacts, low or high EDA, or no SCR).
We performed analyses on the final 60 seconds of each relaxation and film excerpt phase to control for differential stimulus lengths. We removed artifacts (body movements, speech, irregular breathing or disruptions of the skin electrode interface) by visual inspection. We imported data using Ledalab V3.4.3 toolbox (www.ledalab.de/) running on MATLAB 7.7 (MathWorks, Inc.). We ran continuous decomposition analysis (CDA). This method, based on deconvolution, works on the principle that an impulse is followed by a biexponential function (i.e., increased skin conductivity). The automated CDA identifies the impulse and detects the EDA shape, physiologic deviation and interindividual differences. Based on this method, phasic EDA (SCR) can be differentiated more accurately from tonic activity. Moreover, the CDA method is more suitable for long-lasting stimuli and less sensitive to artifacts than other deconvolution methods.
The minimum amplitude criterion for an SCR was 0.05 μS. We summed the amplitudes of the SCRs (i.e., the phasic activity) and extracted the tonic activity. We applied a logarithmic transformation (y = log [1 + x]) to the phasic and tonic data to account for the positive skewed distributions of SCR amplitudes.25 We expressed electrodermal measures using log μS. Because our hypothesis was that apathy would be related to decreased arousal during induction of positive emotion, we assigned positive emotion to tonic and phasic activity during the induction of happiness. In contrast, we had no a priori arguments for choosing specific negative emotions, and were constrained by the small sample sizes. Therefore, we chose to assign negative emotions to the mean of tonic and phasic activities during induction of sadness, fear, anger and disgust. By doing so, positive emotions were related to what is experienced as “pleasant,” and negative emotions were related to what is experienced as “unpleasant.”
Target and nontarget subjective emotional experiences
Positive emotions (e.g., joy) were target items for happiness induction. Negative target items were those that best described the discrete emotion being induced (e.g., “disgusted, turned off, repulsed” was the target item for induction of disgust). Each film excerpt had only 1 target item from the 10 items on the DES; the other 9 were nontargets. For the positive film excerpt, we used the mean of the 9 nontarget items for comparison. For the negative film excerpts, we used the mean of all nontarget items across all 4 negative film excerpts (fear, anger, disgust and sadness). We used the mean of all 4 negative target and nontarget items to score negative subjective emotional experiences. We computed these scores before and after participants viewed the film excerpts.
Statistical analysis
We compared sociodemographic and neuropsychological variables using 1-way analyses of variance (ANOVA; 3 groups). We supplied post hoc comparisons (using a Dunnett test) if main or interaction effects were significant.
We compared clinical variables for the Scz-A and Scz-NA groups using a Student t test. We subjected tonic and phasic EDA measures to repeated-measures ANOVAs (RM-ANOVAs). Two within-participant factors had 2 levels (valence [positive and negative] and induction [relaxation and film viewing]), and 1 between-participant factor had 3 levels (group [controls, Scz-A and Scz-NA]). When RM-ANOVA main effects involving group differences were significant, we ran planned comparisons (defined a priori) for reduced emotional EDA measures in the Scz-A group compared with the other groups. To perform these planned comparisons, we first computed the differences between emotional measures (i.e., tonic and phasic) at baseline38,43 and during the induction phase: for example, emotional measurefilm excerpts – emotional measurebaseline. We then used independent t tests to compare the mean of the variables between the Scz-A group and the control and Scz-NA groups. Planned comparisons increase statistical power by limiting the number of statistical tests that might result from complex factorial designs. As long as the planned comparisons rely on a priori hypotheses and are limited, it is not necessary to adjust for multiple comparison testing.44,45
We performed a multiple linear regression to test for significant association between quantitative apathy measures (AES score) and tonic activity during induction of positive emotions, while accounting for confounding factors.
We used an RM-ANOVA to test for the effectiveness of the battery in individuals and groups in inducing subjective emotional experiences. We used an RM-ANOVA with 3 within-participant factors that had 2 levels (induction [before and after the film excerpt], valence [positive and negative] and item [target and nontarget]), and 1 between-subject factor with 3 levels (group [Scz-A, Scz-NA and control]). For group differences, we tested the main effects of the RM-ANOVA for induction × item × group and induction × item × group × valence. We tested the effectiveness of the battery using the main effect of induction × item. We did not perform post hoc comparisons.
Finally, we used an RM-ANOVA with 1 within-participant factor that had 5 levels (happiness, anger, fear, sadness, disgust) to test for an influence of film excerpt order on EDA measures during relaxation phases in controls.
We performed statistical analysis using SPSS version 22 (IBM Inc.).
Results
Table 1 displays the sociodemographic, clinical and neuropsychological characteristics for each group. We found no statistical differences between groups for age, sex, handedness, educational level or disease duration. We found no significant chlorpromazine-equivalent differences between the Scz-NA and Scz-A groups.
Participant sociodemographic, clinical and neuropsychological characteristics
The findings for tonic and phasic activity, as well as target and nontarget item ratings for each group, are displayed in Table 2.
Tonic and phasic EDA and emotion ratings on target and nontarget scales for positive and negative films*†
Executive function
Although it was not part of our working hypothesis, we found selective executive impairment in initiation (categorical fluency), mental flexibility (TMT), inhibition (Stroop) and strategy switching (Modified Wisconsin Sorting Test) in the Scz-A group compared with the control and Scz-NA groups. Attention was also impaired in the Scz-A and Scz-NA groups (Table 1).
Effectiveness of emotion elicitation procedure
We found a significant induction × item contrast (F1,53 = 118.6, p < 0.001), suggesting a satisfying effect of the battery on the target items, independent of group (i.e., across all individuals; n = 60). We found no group differences in target subjective emotional experiences for induction × item × group (F2,53 = 1, p = 0.7) or induction × item × valence × group (F2,53 = 1.9, p = 0.2). These results suggest that the targeted subjective emotional experiences did not differ between groups after emotional induction (Table 2).
Influence of film order on relaxation phase in controls
To verify that previous emotions did not alter baseline EDA recordings, we ran an RM-ANOVA with 1 within-subject factor that had 5 levels (happiness, anger, fear, sadness, disgust) for both the tonic and the phasic measures. We found no significant effect of emotion for the tonic (F4,16 = 0.7, p = 0.6) or phasic (F4,16 = 0.3, p = 0.8) measure. These nonsignificant results suggest that the order of the film excerpts had no influence on the EDA recordings.
EDA activity
Tonic activity
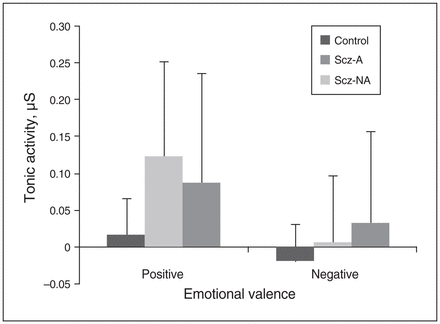
We found significant effects of induction (F1,57 = 12, p = 0.001), induction × valence (F2,57 = 16.1, p < 0.001) and group × induction (F2,57 = 3.3, p = 0.04). We found no effect of valence (F2,57 = 2.4, p = 0.1) or group × valence (F2,57 = 1.3, p = 0.3). We also found no effect of induction × valence × group (F2,57 = 2.2, p = 0.1). To test whether the Scz-A group had reduced tonic activity across valence (i.e., both positive and negative), we first calculated the mean tonic activity between the positive and negative emotions for each participant, and then used planned comparisons to compare tonic activities across emotions between groups. We found decreased tonic activity across emotions (i.e., both positive and negative emotions) in the Scz-A group (mean ± standard deviation [SD] −0.002 ± 0.053) compared with the Scz-NA group (mean ± SD 0.065 ± 0.083, t = 3, p = 0.004) and the control group (mean ± SD 0.06 ± 0.12, t = 2.04, p = 0.048). This revealed significant reduced tonic activity in the Scz-A group across the emotions (i.e., both positive and negative) compared with the Scz-NA and control groups (Fig. 2).
Tonic EDA (μS) in each group during positive and negative film excerpts. Error bars represent standard error of the mean. EDA = electrodermal activity; Scz-A = schizophrena with apathy; Scz-NA = schizophrenia without apathy.
Phasic activity
We found significant effects of induction (F1,57 = 20.7, p < 0.001) and induction × valence (F2,57 = 19.8, p < 0.001). We found no effect of valence (F1,57 = 2.4, p = 0.1). We also found no effect of group × valence (F1,57 = 2.6, p = 0.08), group × induction (F2,57 = 2.5, p = 0.09) or induction × valence × group (F2,57 = 2.3, p = 0.1).
Quantitative apathy as a predictor of tonic EDA activity during induction of positive emotion
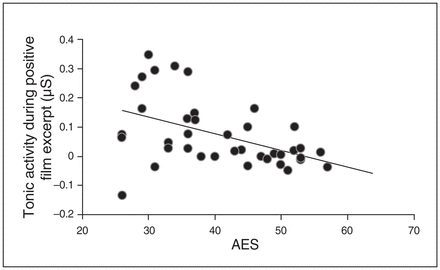
Disease severity, medications and executive dysfunction can confound the relationship between apathy and EDA in schizophrenia. The AES score was highly correlated with the PANSS total score (r = 0.8, p < 0.001), and with the SANS score (r = 0.9, p < 0.001). We did not control for these variables in the linear regression, because it would have violated the assumption of noncollinearity. Instead, we used the PANSS positive subscore to control for the severity of positive symptoms. We conducted a multiple linear regression; the dependent variable was tonic activity during induction of positive emotions, and the independent variables were AES, chlorpromazine equivalent, Wechsler Adult Intelligence Scale digit symbol coding, TMT B–A, categorical fluency (the 3 tests with significant differences between the 3 groups; Table 1) and PANSS positive subscore in the total sample of patients with schizophrenia. Apathy was significantly associated with tonic activity during positive emotions (t = −3.5, p = 0.001), accounting for 24% of the variance (Fig. 3).
Decreased tonic EDA (μS) during the positive film excerpt was associated with higher AES scores. Controlling variables were chlorpromazine equivalents, executive dysfunction and positive PANSS score; β was the standardized estimated coefficient for the AES score. AES = Apathy Evaluation Scale; EDA = electrodermal activity; PANSS = Positive and Negative Syndrome Scale.
Discussion
Using an innovative method to extract tonic and phasic activity from EDA recordings, we tested primarily for decreased tonic activity during induction of positive emotion in Scz-A patients compared with Scz-NA patients and controls. We did not find specific decreased tonic activity during induction of positive emotion in the Scz-A group compared with the Scz-NA group and controls. However, RM-ANOVA revealed a significant effect of group × induction, with decreased tonic activity in Scz-A compared with Scz-NA and controls, independent of valence (i.e., across both positive and negative emotions). Although it was not part of our a priori hypothesis, this result suggested decreased emotion-induced arousal in the Scz-A group versus the Scz-NA group and controls. Using a quantitative measure of apathy in the total sample of schizophrenia patients, we also found that apathy was significantly associated with tonic-related emotional EDA during induction of positive emotion, accounting for 24% of the variance. Our results were consistent with the suggestion that apathy in schizophrenia is associated with reduced emotional experience, especially positive emotion.
We also found impaired executive function in the Scz-A group, in line with previous reports of apathy-related executive impairment in both chronic schizophrenia46 and first episode of psychosis.47 These results support the assessment of apathy in our sample.
Limitations
The first limitation of this study was the lack of a priori estimation of sample size. Indeed, the negative results (i.e., the valence × induction × group interaction) from our primary hypothesis may have stemmed from lack of power, because the quantitative measure of apathy was significantly associated with tonic activity during induction of positive emotion. We are not aware of previous work trying to identify deficits in subjective emotional experiences in schizophrenia relative to apathy, so we were unable to estimate a specific sample size. We based our hypothesis on previous studies that induced emotion in people with schizophrenia using film excerpts and used EDA activities to measure subjective emotional experiences.48
We used only EDA as a physiologic measure of arousal, limiting our conclusions. Future confirmation studies should combine different modalities to quantify arousal.
We induced several emotions sequentially that might have overlapped with each other. This limitation is inherent in all emotion-elicitation paradigms. We added an emotional “washout” period and randomized the order of the film excerpts to limit this possibility. Moreover, post hoc analyses showed no influence of film excerpt order on tonic and phasic measures during relaxation phases in controls. Despite our efforts to reduce the possible overlap of emotion induction, the possibility of overlap should be kept in mind when interpreting our results.
We deliberately avoided assessing apathy in healthy young adults because, from our experience, the AES shows only small variability in this population (data not published).
Participants with schizophrenia were taking antipsychotic and antidepressant medications that might have affected the EDA recordings.49 Antipsychotics can cause hypohidrosis with an antimuscarinic effect and induce lower EDA activity. Antidepressants can cause hyperhidrosis, leading to a noisy signal during EDA recordings. Our ethics committee did not authorize a drug washout period, such as the one in a previous work.48 To limit the potential effect of this issue, we carefully inspected EDA recordings and applied a conservative method of artifact rejection. Moreover, we included the measure of chlorpromazine equivalents in the linear regression, and it was the least significant predictor of tonic activity during positive emotion, explaining only 6.5% of the variance (p = 0.8). This finding suggests that the antimuscarinic effect associated with antipsychotic medications could not explain the difference in EDA recordings during emotion induction in this sample.
We induced more discrete negative emotions (anger, fear, sadness and disgust) than positive emotions (happiness). We averaged the scores for the negative film excerpts and used single scores for the positive excerpt. As a result, the general category of positive emotion was restricted to happiness, and positive emotions were measured with a single estimator, while negative emotions were measured with 4 estimators. Using this approach, we could not form conclusions about differences between positive tonic EDA emotional components and a specific discrete negative tonic EDA emotional component in schizophrenia patients with apathy. As well, we arbitrarily assigned anger, fear, sadness and disgust as “negative” emotions and happiness as a “positive” emotion. Although this seemed intuitive, it was a limitation for the present study.
Conclusion
With the above limitations in mind, the present study yields new insights into the emotional component of apathy in schizophrenia. Alongside the specific cognitive deficits associated with apathy in chronic schizophrenia, our findings provide further arguments for an independent cluster of negative symptoms, namely apathy, associated with altered positive emotions in schizophrenia. Therapeutics that enhance the anticipation of positive emotions could offer new strategies for alleviating apathy in schizophrenia. Our results also point to the need to assess apathy in future studies using EDA (and possibly other psychophysiological recordings) during emotional induction in schizophrenia.
Acknowledgments
The authors would like to thank Dr. Gabrielle Guinard and Dr. Laurine Mégret for their help with recruiting patients. They also thank Stéphane Brousse and Jacques Soulabaille for their help with recruiting healthy controls. This work is dedicated to the memory of Nicolas Hervé, who passed away during the preparation of this work. He contributed to the analysis of EDA data. He will be missed by all his colleagues from the Guillaume Régnier Hospital in Rennes.
Footnotes
Competing interests: None declared.
Funding: This work was supported by an internal grant promoted by the Guillaume Régnier Hospital.
Contributors: T. Dondaine, J.-M. Batail, F. Le Jeune, S. Drapier, B. Millet, D. Drapier and G. Robert designed the study. T. Dondaine acquired and analyzed the data, which P. Philippot, P. Sauleau, M. Vérin, D. Drapier and G. Robert analyzed. T. Dondaine wrote the article, which all authors reviewed. All authors approved the final version to be published and can certify that no other individuals not listed as authors have made substantial contributions to the paper.
- Received August 29, 2017.
- Revision received January 10, 2018.
- Revision received May 14, 2018.
- Accepted May 22, 2018.