Abstract
The addition of low doses of atypical antipsychotic drugs, which saturate 5-HT2A receptors, enhances the therapeutic effect of selective serotonin (5-hydroxytryptamine; 5-HT) reuptake inhibitors (SSRIs) in patients with major depression as well as treatment-refractory obsessive-compulsive disorder. The purpose of the present studies was to test the effects of combined treatment with a low dose of a highly selective 5-HT2A receptor antagonist (M100907; formerly MDL 100,907) and low doses of a SSRI using a behavioral screen in rodents (the differential-reinforcement-of low rate 72-s schedule of reinforcement; DRL 72-s) which previously has been shown to be sensitive both to 5-HT2 antagonists and SSRIs. M100907 has a ∼100-fold or greater selectivity at 5-HT2A receptors vs other 5-HT receptor subtypes, and would not be expected to appreciably occupy non-5-HT2A receptors at doses below 100 μg/kg. M100907 increased the reinforcement rate, decreased the response rate, and shifted the inter-response time distributions to the right in a pattern characteristic of antidepressant drugs. In addition, a positive synergistic interaction occurred when testing low doses of the 5-HT2A receptor antagonist (6.25–12.5 μg/kg) with clinically relevant doses of the SSRI fluoxetine (2.5–5 mg/kg), which both exerted minimal antidepressant-like effects by themselves. In vivo microdialysis study revealed that a low dose of M100907 (12.5 μg/kg) did not elevate extracellular 5-HT levels in the prefrontal cortex over those observed with fluoxetine alone (5 mg/kg). These results will be discussed in the context that the combined blockade of 5-HT2A receptors and serotonin transporters (SERT) may result in greater efficacy in treating neuropsychiatric syndromes than blocking either site alone.
Similar content being viewed by others
INTRODUCTION
Blockade of the serotonin (5-hydroxytryptamine; 5-HT) transporter (SERT) is the common pharmacological action shared by selective serotonin reuptake inhibitors (SSRIs; eg citalopram, escitalopram, fluoxetine, fluvoxamine, paroxetine, sertraline), approved by regulatory agencies for the treatment of mood and anxiety disorders. Enhancement of 5-HT synaptic availability appears to be a critical component of the mechanism underlying the action of SSRIs in the treatment of depression as demonstrated by the tryptophan depletion paradigm (Delgado et al, 1990, 1999). However, there are at least 14 known 5-HT receptors in the brain (excluding splice variants and edited isoforms). Remarkably little is known regarding which 5-HT receptors are involved (positively and negatively) in the therapeutic effects of SSRIs over a diverse range of neuropsychiatric syndromes such as major depression, bipolar depression, obsessive-compulsive disorder (OCD), panic disorder, generalized anxiety disorder (GAD), post-traumatic stress disorder (PTSD), social anxiety disorder, and pervasive developmental disorders.
A growing body of clinical psychopharmacological evidence is consistent with the hypothesis that blockade of 5-HT2A receptors might enhance the therapeutic effectiveness of SSRIs. First and foremost, a number of placebo-controlled trials have found that addition of drugs, which share a common pharmacological action of 5-HT2 receptor blockade (eg, mianserin, mirtazapine, and olanzapine), appear to enhance the antidepressant efficacy of SSRIs (Marek et al, 2003). Several open-label reports have further suggested that low doses of the atypical antipsychotic drug risperidone (0.5–1 mg/day), which shows ∼30-fold 5-HT2A vs 5-HT2C selectivity, results in a rapid decrease in depressive symptoms in depressed patients when initiated with SSRI treatment or when added to ongoing SSRI treatment (Hirose and Ashby, 2002; O'Connor and Silver, 1998; Ostroff and Nelson, 1999). These studies would be consistent with the hypothesis that activation of 5-HT2A receptors acts in opposition to activation of critical non-5-HT2A receptors and the cascade of events leading to therapeutic efficacy.
One strategy to explore potential 5-HT receptor interactions is to study animal models of depression or antidepressant drug screens. The differential-reinforcement-of low rate 72-s (DRL 72-s) schedule is a screen for antidepressant drugs that is sensitive both to 5-HT2 receptor antagonists and SSRIs (Marek and Seiden, 1988; Seiden et al, 1985; Sokolowski and Seiden, 1999). Rats performing under a DRL 72-s schedule are required to withhold responses for at least 72 s following the previous response in order to receive a reinforcer. Theoretically, drugs may increase the number of reinforcers obtained and induce rightward shifts in inter-response time (IRT) distributions in rats performing under a DRL 72-s schedule by either altering temporal discrimination or enhancing the ability of rats to withhold inappropriate responses (O'Donnell et al, 2005).
The first purpose of the present studies, given the considerable pharmacological overlap between different members of the 5-HT2 family of receptors, was to test for antidepressant-like effects on the DRL 72-s schedule of a highly selective 5-HT2A receptor antagonist (M100907; formerly MDL 100,907), at doses that are known to be selective for the 5-HT2A receptor (Kehne et al, 1996). The second purpose was to test whether a synergistic interaction may occur on DRL 72-s behavior between a 5-HT2A receptor antagonist and an SSRI by examining administration of several doses of M100907 and fluoxetine that are relatively inactive alone. Third, an in vivo dialysis study was conducted to examine whether administration of relatively low doses of the 5-HT2A receptor antagonist M100907 elevated prefrontal extracellular 5-HT levels over that seen with fluoxetine administration.
MATERIALS AND METHODS
Subjects
A total of 23 male Sprague–Dawley rats weighing between 300 and 350 g at the beginning of the behavioral experiments (Holtzman, Madison, WI) were housed in suspended stainless steel wire cages (18 × 36 × 20 cm) with two rats occupying each cage. The colony room was maintained at 20°C and relative humidity (60%). The room was illuminated 12 h/day (0700–1900 hours). All rats had free access to laboratory chow (Teklad 4% Rat Diet) except during experimental sessions. Water was available for a 20 min period following the daily behavioral session. The principles of laboratory animal care (NIH publication No. 85–23, revised 1985) were followed.
In total,24 male albino Wistar rats (Iffa Credo, Lyon, France) weighing 280–320 g were employed for the in vivo microdialysis experiments. The colony room was maintained at 22±2°C. Food and water were provided ad libitum before and during experiments. Animal care followed the European Union Regulations (O.J. of E.C. L358/1 18/12/1986) and procedures were approved by the local Ethics Committee.
Apparatus
Eight MED Associates operant-conditioning chambers (30.5 × 24.1 × 29.2 cm; St Albans, VT; www.med-associates.com) were used for the DRL experiments. The lever in these chambers was mounted on one wall with the water access next to the lever in the middle of the wall. A reinforced response caused the dipper (0.02 cc cup) to be lifted from a water trough to an opening in the floor of the access port for 4 s. The houselight (which was mounted on the opposite wall) was turned on when the session began, remained on throughout the entire session and turned off at the end of the session. Each experimental chamber was enclosed in a melamine sound-attenuating cubicle and equipped with a white noise generator to provide masking noise.
Operant Training
Rats were water deprived for ∼22.5 h before each session. Each rat was initially trained under an alternative fixed ratio 1, fixed-time 1 min schedule for water reinforcement. Thus, each response was reinforced and water was also provided every minute if a response did not occur. The few rats that did not acquire lever-pressing behavior after three daily 1 h sessions under this schedule were trained by the experimenter using the method of successive approximation. After the rats had acquired lever-pressing behavior, they were trained during daily DRL 18-s sessions for ∼2 weeks before moving directly to DRL 72-s sessions. The responding on these sessions became stable after ∼8 weeks. Experimental sessions lasted for 1 h and were conducted 5 days/week during light hours.
Surgery and Microdialysis Procedures
An updated description of the microdialysis procedures has been published (Adell and Artigas 1998). Rats were anesthetized with pentobarbital (60 mg/kg i.p.) and concentric dialysis probes were implanted in the prefrontal cortex (PFC). Two different locations were chosen to target mainly layers 3–5 (medial PFC, mPFC) and layer 6 (lateral PFC, lPFC). Probes were secured to the skull with anchor screws and dental cement. Dialysis membranes were made from hollow Cuprophan fibers with 252 μm OD, 220 μm ID, and a nominal 5000-Da molecular weight cutoff (GFE09, Gambro, Lund, Sweden). The active zone in the probes was 4 mm long. The stereotaxic coordinates were AP +3.4, DV −6.0; L −0.8 (mPFC) or L −2.5 mm (lateral PFC; lPFC). They were taken from bregma and dura mater according to the rat brain atlas of Paxinos and Watson (1986). Another group of rats was implanted with probes in the dorsal striatum (AP +0.2, DV −8.0, L −3.0). Rats were allowed to recover from anesthesia in the dialysis cages (cubic, 40 cm each side) and 20–24 h later the probes were perfused with artificial CSF (aCSF; composition: NaCl 125 mM, KCl 2.5 mM, MgCl2 1.18 mM, and CaCl2 1.26 mM; pH 6.5–7.0) at 1.5 μl/min. Dialysate samples of 30 μl were collected at 20-min intervals into polypropylene microcentrifuge vials. After an initial 1 h, sample of dialysate was discarded, four fractions were collected to obtain basal values before drug administration. At the end of the experiments, rats were killed by an overdose of sodium pentobarbital. The placement of the dialysis probes was checked by perfusing Fast Green dye and examination of the probe track after cutting the brain at the appropriate level. Only animals with probes correctly placed were included in the calculations.
5-HT was analyzed by a modification of a high-performance liquid chromatography method previously described in an updated form (Adell and Artigas, 1998). 5-HT was separated on a 3 μm ODS 2 column (7.5 cm × 0.46 cm; Beckman, San Ramon, CA) and detected amperometrically with a Hewlett Packard 1049 detector set at the potential of +0.6 V. Retention time was 3.5–4 min. The detection limit for 5-HT was typically 1 fmol/sample. Dialysate 5-HT values were calculated by reference to standard curves run daily.
Schedule Control and Statistical Analyses
The experimental chambers were connected to a PC via an MED-SYS-8 interface and software package. All behavioral data are expressed as the mean±SEM normalized to the vehicle or vehicle–vehicle condition. The data analysis was performed on the raw data. The effects of M100907 (3.25–100 μg/kg) and fluoxetine (2.5–10 mg/kg) alone were analyzed with a one-factor repeated measures analysis of variance (ANOVA). The effects of the combined treatment of M100907 and fluoxetine were analyzed with a two-factor repeated measures AOVA using M100907 and fluoxetine as within-subject factors. Significant main effects or interactions were analyzed by the Newman–Keuls or Dunnett test, where appropriate. The level of significance was set for p<0.05 for all analyses.
The IRT distribution for each individual rat was analyzed with the nonparametic Kolmogorov–Smirnov test to make within-subject comparisons between different treatment conditions. The level of significance was conservatively set for p<0.001, even though only a limited set of a priori comparisons were planned.
Microdialysis results are expressed as femtomoles per fraction (uncorrected for recovery) and shown in figures as percentage of basal values (individual means of four predrug fractions). Statistical analysis of drug effects on dialysate 5-HT was performed using one-or two-factor repeated measures ANOVA with time as the repeated factor and drug as an independent factor.
Drugs
Doses were calculated on the basis of the salt forms. The drugs were dissolved in saline, neutralized to a pH∼7.4, and injected i.p. in a volume of 1 ml/kg body weight. M100907 was a gift from Marion Merrell Dow (Cincinnati, OH; now Sanolfi-Aventis) and fluoxetine was a gift from Eli Lilly and Company (Indianapolis, IN). Drugs were administered to the animals only once weekly in an ascending order of dose magnitiude (Thursday) to minimize possible carryover effects since a majority of 5-HT2A receptor antagonists have been associated with 5-HT2A receptor downregulation. In experiments where both fluoxetine and M100907 were administered, dose–response determinations for fluoxetine alone and M100907 alone were obtained concurrently with the combination such that fluoxetine 10 mg/kg–vehicle, vehicle–M100907 (25 mg/kg), and vehicle–M100907 (50 mg/kg) were examined after all combinations of the two drugs had been tested. Behavior returned to baseline the day following drug administration.
RESULTS
Antidepressant-Like Action of M100907 on DRL 72-s Behavior
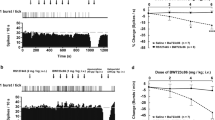
Since most atypical antidepressants (which do not appreciably block monoamine uptake or monoamine oxidase, MAO) share considerable potency at both 5-HT2A and 5-HT2C receptors, we examined a highly selective antagonist for 5-HT2A vs 5-HT2C receptors. M100907 exerted a dose-dependent (3.12–1000 μg/kg, i.p.) increase in the reinforcement rate (F(8,40)=5.83, p<0.001; Figure 1) and decrease in the total response rate (F(8,40)=3.89, p<0.01; Figure 1), similar to the effects of tricyclic antidepressants. The ED50 for the changes in the reinforcement and response rates was ∼12 μg/kg calculated by nonlinear curve fitting (Delta Graph, not shown). The maximal increase in the reinforcement rate and decrease in the response rate occurred at 100 μg/kg. Interestingly, the magnitude of changes in the reinforcement and response rate was numerically smaller at the 300 and 1000 μg/kg doses than the 100 μg/kg dose. Overall, there appears to be pproximately a 25-fold selectivity between the ED50 for increasing the reinforcement rate and the first dose of M100907 with an appreciable submaximal effect (300 μg/kg, i.p.).
Dose-dependent changes in the frequency of reinforcers and total responses induced by the 5-HT2A receptor antagonist M100907 (3.13–1000 μg/kg, i.p.) for male Sprague–Dawley rats performing on a DRL 72-s schedule. The increased reinforcement rate is shown in squares, while the decreased response rate is displayed with circles. For the vehicle–vehicle condition, the mean (±SEM) number of reinforcers obtained was 10.6 (±2.2), while the mean (±SEM) number of total responses was 74.9 (±8.2). Rats were injected (i.p.; 1 ml/kg, n=7) 1 h prior to a 1 h behavioral session. The maximal change in the reinforcement and total response rate occurred at the 100 μg/kg dose, while the ED50 for the increase in the reinforcement rate was 12 μg/kg (Delta Graph, not shown). Significant changes from the vehicle control are indicated for p<0.05, * and p<0.01, **.
Examination of the IRT distributions revealed that M100907 resulted in a cohesive shift to the right in the IRT distribution (Figure 2), similar to the effects of TCAs, MAOIs, and atypical antidepressants. Compared to the vehicle condition, a significantly different IRT distribution (p<0.001, Kolmogorov–Smirnov test) with an increased mean IRT was associated with the following M100907 doses (6.25 μg/kg, one of eight rats; 12.5 μg/kg, one of eight; 25 μg/kg, two of eight; 50 μg/kg, three of eight; 100 μg/kg, four of eight; 300 μg/kg, three of eight; 1000 μg/kg, zero of eight).
Effects of the selective 5-HT2A receptor antagonist M100907 (25–100 μg/kg) on inter-response time (IRT) distributions for rats performing on a DRL 72-s schedule. The effects for two rats are shown where a rightward shift (typical of most antidepressant drugs) in the IRT distribution occurred compared to the vehicle condition. For rat 61 and 65, significant changes from the vehicle condition occurred at each of the three doses shown (p<0.001, Kolmogorov–Smirnov test). The mean IRT for the conditions shown for rat 61 was 46.6 s (vehicle, SD 30.7); 72.5 (25 μg/kg, SD 49.9); 68.4 (50 μg/kg, SD 30.7); 124.1 (100 μg/kg, SD 118.1). The mean IRT for the conditions shown for rat 65 was 55.2 s (vehicle, SD 18.0); 71.2 (25 μg/kg, SD 22.1); 71.7 (50 μg/kg, SD 22.0); 78.6 (100 μg/kg, SD 21.0).
Interaction between M100907 and Fluoxetine on DRL 72-s Behavior
We next examined the interaction of low doses of both M100907 and fluoxetine using a different group of eight subjects in order to specifically test for an interaction between the effects of simultaneously blocking 5-HT2A receptors and SERT. Fluoxetine (2.5–10 mg/kg, i.p.) exerted significant increases in the reinforcement rate (F(3,21)=10.59, p<0.001; Figure 3) only at the highest dose tested (226±25.2% of vehicle control; mean±SEM; not shown) consistent with previous results. Higher doses were not tested as the 10 mg/kg dose appears to result in maximal effects on DRL behavior as it also does for elevation of prefrontal extracellular 5-HT levels (Hervas and Artigas, 1998). Fluoxetine alone did not significantly reduce the total response rate (Figure 3; F(3,21)=1.85, p=0.17).
Dose-dependent changes in the frequency of reinforcers (top) and responses (bottom) induced by combinations of the 5-HT2A receptor antagonist M100907 (6.25 or 12.5 μg/kg or vehicle, i.p.) and fluoxetine (2.5 or 5 mg/kg or vehicle) for rats (n=8) performing on a DRL 72-s schedule. For the vehicle–vehicle condition, the mean (±SEM) number of reinforcers obtained was 6.5 (±0.9). For the vehicle–vehicle condition, the mean (±SEM) number of total responses made was 88 (±3.7). Rats were injected (i.p.; 1 ml/kg, n=8) 1 h prior to a 1 h behavioral session. Significant changes from the vehicle control are indicated for p<0.05, * and p<0.01, **. Significant changes from the respective M100907-vehicle or vehicle–fluoxetine condition were indicated by either ‘m’ or ‘f’ for p<0.05.
Typical examples for the effects of fluoxetine on the IRT distribution are shown for several rats in Figure 5. Compared to the vehicle–vehicle condition, no effects were observed on the IRT distributions for most of the subjects. Significant differences in the IRT distribution associated with an increased mean IRT occurred in 0, 0, and two rats (out of eight total) for the 2.5, 5, and 10 mg/kg fluoxetine doses, respectively. Significant differences in the IRT distribution (associated with a decreased mean IRT) occurred only at the 2.5 mg/kg dose where three out of eight subjects had a significant change in the IRT distribution compared to the control condition where there was a decrease in the mean IRT.
Effects of the selective 5-HT2A receptor antagonist M100907 (12.5 μg/kg) or vehicle and fluoxetine (5 mg/kg) or vehicle on inter-response time (IRT) distributions for rats performing on a DRL 72-s schedule. The effects for two rats are shown where a significant rightward shift (typical of most antidepressant drugs) in the IRT distribution occurred in the M100907+fluoxetine condition compared to the other three conditions (p<0.001, Kolmorgorov–Smirnov test). The mean IRT for the conditions shown for rat 74 were 47.4 s (vehicle–vehicle, SD 25.3); 45.6 (fluoxetine, 5 mg/kg+vehicle, SD 27.0); 49.8 (vehicle+M100907, 12.5 μg/kg, SD 27.4); 68.7 (fluoxetine, 5 mg/kg+M100907, 12.5 μg/kg, SD 35.5). The mean IRT for the conditions shown for rat 77 was 42.6 s (vehicle–vehicle, SD 18.5); 41.8 (fluoxetine, 5 mg/kg+vehicle, SD 23.1); 39.8 (vehicle+M100907, 12.5 μg/kg, SD 20.8); 56.3 (fluoxetine, 5 mg/kg+M100907, 12.5 μg/kg, SD 31.7).
The maximal dose of M100907 tested for animals used in the drug interaction experiment was 50 μg/kg. There was a significant overall effect for M100907 on the reinforcement rate (Figure 3; F(4,28)=3.39, p<0.05) but not the response rate (Figure 3; F(4,28)=1.90, p=0.14). The lowest two doses (6.12 and 12.5 μg/kg) did not significantly alter the behavior of the rats performing on the DRL 72-s schedule. Higher doses (25 and 50 μg/kg, i.p., not shown) did significantly increase the reinforcement rate (171±18 and 165±26% of vehicle–vehicle control, respectively) and nonsignificantly decreased the response rate (93±5 and 93±8% vehicle–vehicle control, respectively).
The combined administration of M100907 and fluoxetine resulted in substantial increases in the reinforcement rate and decreases in the response rate that were greater than the combined effects of the two drugs independently. For the reinforcement rate, significant main effects of M100907 (F(2,14)=45.15, p<0.001) and fluoxetine (F(2,14)=31.43, p<0.001) were present together with a significant interaction effect (F(4,28)=3.63, p<0.05). Three of the four combined doses of the two drugs tested (M100907, 6.25 μg/kg+fluoxetine, 5 mg/kg; M100907, 12.5 μg/kg+fluoxetine, 2.5 mg/kg; M100907, 12.5 μg/kg+fluoxetine, 5 mg/kg) were significantly different from the effects of both the respective dose of M100907 alone or fluoxetine alone (Newman–Keuls, p<0.01).
For the total response rate, significant main effects of M100907 (F(2,14)=4.16, p<0.05) and fluoxetine (F(2,14)=6.28, p<0.05) and a significant interaction effect (F(4,28)=8.41, p<0.001) were present (Figure 4). All four combined doses of these two drugs tested were significantly different from the effects of the respective M100907 or fluoxetine dose alone or the vehicle–vehicle condition (p<0.05) except for the combination of M100907 (12.5 μg/kg) and fluoxetine (2.5 mg/kg).
Effects of the SSRI fluoxetine (2.5–10 mg/kg) on inter-response time (IRT) distributions for rats performing on a DRL 72-s schedule. For rats 75 and 77, no significant changes from the vehicle condition occurred for the three doses shown (p<0.001, Kolmogorov–Smirnov test). The 5 mg/kg dose administered to rat 75 exhibited a trend towards a significant difference from the vehicle control with an decreased mean IRT (p<0.005). The mean IRT for the conditions shown for rat 75 was 65.5 s (vehicle, SD 22.6); 61.0 (2.5 mg/kg, SD 18.8); 55.3 (5 mg/kg, SD 19.5); 62.1 (10 mg/kg, SD 15.8). The mean IRT for the conditions shown for rat 77 was 42.6 s (vehicle, SD 18.5); 34.0 (2.5 mg/kg, SD 25.0); 41.8 (5 mg/kg, SD 23.1); 45.3 (10 mg/kg, SD 25.2).
The comparison of the IRT distributions for the combination of M100907 and fluoxetine vs the vehicle–vehicle condition confirms the synergistic interaction between these two drugs (Figures 4 and 5). This synergistic interaction was most apparent for the combination of the highest dose of M100907 and fluoxetine tested where four of eight rats had an IRT distribution that was significantly different (p<0.001, Kolmogorov–Smirnov test; and associated with an increased mean IRT) than the vehicle–vehicle condition. In contrast, only one of eight subjects administered the same 12.5 μg/kg dose of M100907 alone had a significantly different IRT distribution than the vehicle–vehicle condition, and in this subject the mean IRT was decreased. None of eight subjects administered fluoxetine (5 mg/kg) had a significantly different IRT distribution that was associated with an increased mean IRT compared to the vehicle–vehicle condition (Figure 4). Furthermore, five of eight rats administered the combination of M100907 (12.5 μg/kg) and fluoxetine (5 mg/kg) had a significantly different IRT distribution (associated with an increased mean IRT) compared to the vehicle–fluoxetine (5 mg/kg) condition. Similarly, four of eight rats administered the combination of M100907 (12.5 μg/kg) and fluoxetine (5 mg/kg) had a significantly different IRT distribution (associated with an increased mean IRT) compared to the M100907 (12.5 μg/kg)–vehicle condition.
This apparent synergistic effect between fluoxetine and M100907 on the IRT distributions was also highlighted by comparison of the M100907 (12.5 μg/kg)–fluoxetine (2.5 mg/kg) condition to the vehicle–vehicle condition or the vehicle–fluoxetine (2.5 mg/kg) condition (not shown). While the vehicle–fluoxetine (2.5 mg/kg) condition was associated with three of eight rats demonstrating significant changes (p<0.001, Kolmogorov–Smirnov test) in the IRT distribution compared to the vehicle–vehicle condition (decreased mean IRT), the combination of M100907 (12.5 μg/kg) and fluoxetine (2.5 mg/kg) was associated with four of eight rats, demonstrating significant changes in the IRT distribution compared to the vehicle–vehicle condition (increased mean IRT). While only one of eight rats demonstrated a significant change (p<0.001) in the IRT distribution for the M100907 (12.5 μg/kg)–fluoxetine (2.5 mg/kg) condition compared to the M100907 (12.5 μg/kg)–vehicle condition (associated with an increased mean IRT), an additional four of eight subjects administered the combination of M100907 (12.5 μg/kg) and fluoxetine (2.5 mg/kg) exhibited a trend towards a significantly different IRT distribution (p<0.005, associated with an increased mean IRT).
A replication of this experiment in a second group of subjects confirmed that there was at least an additive antidepressant-like effect of the M100907 and fluoxetine in rats performing on the DRL 72-s schedule. Fluoxetine (2.5–10 mg/kg) did not significantly increase the reinforcement rate or decrease the response rate, although the reinforcement rate was nonsignificantly increased to 149% of control at the 5 (Table 1) and 10 mg doses (not shown). M100907 (6.25–50 μg/kg) did not significantly increase the reinforcement rate but did significantly decrease the response rate (F(4,28)=6.62). When examining the effects of M100907 (6.25–12.5 μg/kg) and fluoxetine (2.5–5 mg/kg), a significant main effect for fluoxetine (F(2,14)=5.28, p<0.05) and M100907 (F(2,14)=8.33, p<0.01) and a trend towards an interaction effect (F(4,28)=2.51, p=0.06) on reinforcers were observed. The only data points significantly different from the vehicle–vehicle condition were for the M100907 (6.25 μg/kg)–fluoxetine (2.5 mg/kg); M100907 (6.25 μg/kg)–fluoxetine (5 mg/kg); and M100907 (12.5 μg/kg)–fluoxetine (5 mg/kg) combinations. The combination of the higher doses of M100907 and fluoxetine tested were also significantly greater than the M100907 (12.5 μg/kg)–vehicle condition or the vehicle–fluoxetine (5 mg/kg) condition.
When examining the effects of M100907 (6.25–12.5 μg/kg) and fluoxetine (2.5–5 mg/kg) on the total response rate, a significant main effect for M100907 (F(2,14)=17.61, p<0.001), but not for fluoxetine (p<0.1), was observed (Table 2). The interaction effect was not significant.
The comparison of the IRT distributions for the combination of M100907 and fluoxetine vs the vehicle–vehicle condition in this second group of subjects, like in the previous group, suggests a synergistic interaction between these two drugs (Figure 6). Thus, all eight rats administered the combination of M100907 (12.5 μg/kg) and fluoxetine (5 mg/kg) had an IRT distribution that was significantly different (p<0.001, and associated with an increased mean IRT) than the vehicle–vehicle condition. In contrast, zero of eight subjects administered the same 12.5 μg/kg dose of M100907 alone had a significantly different IRT distribution than the vehicle–vehicle condition. Only two of eight subjects administered fluoxetine (5 mg/kg) had a significantly different IRT distribution (associated with an increased mean IRT) compared to the vehicle–vehicle condition. Furthermore, three of eight rats administered the combination of M100907 (12.5 μg/kg) and fluoxetine (5 mg/kg) had a significantly different IRT distribution (associated with an increased mean IRT) compared to the vehicle–fluoxetine (5 mg/kg) condition. Similarly, three of eight rats administered the combination of M100907 (12.5 μg/kg) and fluoxetine (5 mg/kg) had a significantly different IRT distribution (associated with an increased mean IRT) compared to the M100907 (12.5 μg/kg)–vehicle condition.
Effects of the selective 5-HT2A receptor antagonist M100907 (12.5 μg/kg) or vehicle and fluoxetine (5 mg/kg) or vehicle on inter-response time (IRT) distributions for several rats from a second group performing on a DRL 72-s schedule. The effects for two rats are shown where a significant rightward shift (typical of most antidepressant drugs) in the IRT distribution occurred in the M100907+fluoxetine condition compared to the other three conditions (p<0.001, Kolmorgorov–Smirnov test). The mean IRT for the conditions shown for rat 84 were 53.1 s (vehicle–vehicle, SD 18.7); 56.1 (fluoxetine, 5 mg/kg+vehicle, SD 24.6); 56.9 (vehicle+M100907, 12.5 μg/kg, SD 29.0); 78.1 (fluoxetine, 5 mg/kg+M100907, 12.5 μgkg, SD 32.4). The mean IRT for the conditions shown for rat 85 were 35.1 s (vehicle–vehicle, SD 22.1); 33.5 (fluoxetine, 5 mg/kg+vehicle, SD 20.3); 36.4 (vehicle+M100907, 12.5 μg/kg, SD 23.9); 53.6 (fluoxetine, 5 mg/kg+M100907, 12.5 μg/kg, SD 29.9).
5-HT Levels: In Vivo Microdialysis Experiments Following Fluoxetine and M100907
Fluoxetine (5 mg/kg, i.p.) increased the extracellular concentrations of 5-HT in prefrontal cortex (Figure 7) as previously observed (Hervas and Artigas 1998). Since extracellular 5-HT concentrations have been reported only for a possibly nonselective dose of M100907 (1000 μg/kg, i.p.) after fluoxetine administration (Zhang et al, 2000), we chose to examine 5-HT levels following a low dose of M100907 (12.5 μg/kg) which had a synergistic behavioral interaction with fluoxetine. M100907 did not increase extracellular 5-HT concentrations following fluoxetine compared to a saline-treated control group (eg, fluoxetine-saline) in the medial or lateral prefrontal cortex (Figure 7). Two-way ANOVA of these data revealed a significant effect of time in both areas (F15,90=18.0, p<0.00001 in medial prefrontal cortex; F15,90=12.9, p<0.000001 in lateral prefrontal cortex) but not of the group or time × group interaction. An increase in extracellular 5-HT levels was observed after the administration of saline and M100907, which is possibly related to the injection-associated stress. Similar results were also observed for the interaction of M100907 and fluoxetine in the striatum (not shown).
Effects of the SSRI fluoxetine (5 mg/kg) and M100907 (12.5 μg/kg) or saline on 5-HT in dialysates from the mPFC (a) and lPFC (b). All rats were administered fluoxetine (first arrow) after measuring stable baseline over four 20 min fractions. Fluoxetine elicited a stable increase of the extracellular 5-HT concentration in both areas. After 2 h, rats were injected i.p. with saline (open circles) or M100907 (filled circles) (second arrow). The injection of saline and M100907 induced a transient increase in 5-HT, which is most likely associated to the stress of handling the rats and the injection itself. Data are means±SEM of 4–5 rats/group.
DISCUSSION
The main finding from the present study using the DRL 72-s schedule is that simultaneous blockade of 5-HT2A receptors and SERT results in antidepressant-like efficacy (increased reinforcement rate, decrease in response rate, and a rightward shift in the IRT distribution) of greater magnitude than would be expected from the additive effects of either drug administered alone. The most prominent evidence of a synergistic interaction between M100907 and fluoxetine was found for effects on the IRT distributions, while the synergistic effect on the number of reinforcers obtained was obvious in only one of two separate groups of subjects tested.
The use of the highly selective 5-HT2A receptor antagonist M100907 (Kehne et al, 1996) confirmed previous suggestions that selective blockade of 5-HT2A relative to 5-HT2C or other receptors pharmacologically similar to the 5-HT1 receptor family results in antidepressant-like effects on the DRL 72-s schedule (Marek and Seiden, 1988; Marek et al, 1989; Marek and Seiden, 1994). The present results are in contrast to a popular antidepressant drug screen, the forced swim or Porsolt test, where selective 5-HT2A antagonists do not decrease immobility similar to most antidepressant drugs (Luttinger et al, 1985; Borsini, 1995). Furthermore, the 5-HT2A antagonist ketanserin failed to potentiate the anti-immobility effect for subactive doses of fluoxetine, citalopram, or fluvoxamine in the mouse forced swim test (Redrobe and Bourin, 1997). However, a recent report that swim stress induces a profound suppression of head shakes induced by 5-HT2A receptor activation seriously questions whether negative effects of 5-HT2A antagonists on the forced swim test might represent a false negative result due to a physiological confound with this paradigm (Pericic, 2003).The present antidepressant-like effects of M100907 both alone and in combination with the SSRI fluoxetine are probably mediated by blockade of central 5-HT2A receptors. Although M100907 was not administered centrally, previously a highly selective 5-HT2 receptor antagonist lacking CNS penetrance (xylamidine) failed to exert an antidepressant-like effect on DRL 72-s behavior (Marek et al, 1989). The high potency of M100907 on DRL 72-s behavior is in excellent agreement with the high potency of M100907 (ED50=5 μg/kg) in blocking DOI-induced head shakes in the rat (Schreiber et al, 1995). The present M100907 data are an important extension of previous pharmacological studies using the DRL 72-s schedule as this drug does not possess potent α1-adrenergic blockade and also does not bind to the tetrabenazine-sensitive vesicular sites or 5-HT1D receptors as one of the previously tested 5-HT2A antagonists, ketanserin. Nevertheless, the numerically inferior performance of higher M100907 doses (0.3 and 1.0 mg/kg) compared to the maximal changes in reinforcement and response rate at 0.1 mg/kg may reflect decreased pharmacological specificity at these higher doses such as 5-HT2C receptors (Kehne et al, 1996; Marek and Seiden, 1994) or a preferential activation of a subpopulation of 5-HT2A receptors in different cellular compartments and/or phenotypes (Aghajanian and Marek, 1997; Jakab and Goldman-Rakic, 1998, 2000; Miner et al, 2003; Willins et al, 1997; Zhou and Hablitz, 1999). Other investigators have reported that 5-HT2C receptor agonist activity is associated with increases in the reinforcement rate and decreases in the response rate in rats performing on a DRL 72-s schedule (Martin et al, 1998), thus blockade of 5-HT2C receptors may counter ‘antidepressant-like’ effects of 5-HT2A receptor antagonists on DRL 72-s behavior.
The apparent synergistic effects of M100907 and fluoxetine on rats performing on the DRL 72-s schedule argue for a pharmacodynamic rather than a pharmacokinetic mechanism underlying this behavioral drug–drug interaction. The lack of an effect of M100907 on the fluoxetine (5 mg/kg, ip)-induced increase in extracellular 5-HT in both the prefrontal cortex and striatum is not consistent with M100907 altering fluoxetine metabolism. However, drug levels for fluoxetine and M100907 were not analyzed to rule out such a pharmacokinetic interaction.
To our knowledge, this represents the first preclinical report suggesting that selective blockade of 5-HT2A receptors may have a synergistic effect with blockade of SERT. SSRIs have minimal effects on the IRT distribution that appears to be qualitatively different from the cohesive rightward shifts induced by TCAs, MAOIs, and atypical antidepressants (O'Donnell and Seiden, 1982; Richards and Seiden, 1991; Seiden et al, 1985; Sokolowski and Seiden, 1999). In contrast, the effects of selective 5-HT2A receptor blockade on IRT distributions of rats performing on the DRL 72-s schedule appears qualitatively similar to TCAs, MAOIs, and ‘atypical’ antidepressants (which do not appreciably block monoamine transporters or MAO). The rightward shifts in the IRT distribution were most marked for the combinations of M100907 and fluoxetine. The absence of an interaction of fluoxetine and M100907 at increasing extracellular 5-HT in the mPFC, lateral prefrontal cortex, and striatum is not consistent with the hypothesis that a synergistic increase in extracellular 5-HT is the pharmacodynamic mechanism mediating the synergistic behavioral effect of the 5-HT2A antagonist and the SSRI. These present in vivo dialysis results obtained in Wistar rats with a lower dose of M100907 are similar to past results obtained with a higher dose of M100907 (1 mg/kg, s.c.) in Sprague–Dawley rats (Zhang et al, 2000).
The present behavioral interactions between 5-HT2A receptor blockade and SERT inhibition on DRL behavior would appear consistent with the general excitatory actions of 5-HT2A receptors and inhibitory effects of 5-HT1-like receptors in areas such as the mPFC and neocortex. Activation of 5-HT2A receptors depolarizes pyramidal neurons (Araneda and Andrade, 1991; Tanaka and North, 1993) and enhances their firing activity (Puig et al, 2003), an effect that may involve glutamate release from thalamocortical afferents (Marek et al, 2001). In contrast, activation of 5-HT1A receptors hyperpolarizes pyramidal neurons (Araneda and Andrade, 1991; Ashby et al, 1994) and activation of 5-HT1B/1D heteroceptors can decrease release of glutamate and/or other excitatory amino acids (Marcoli et al, 1999; Maura et al, 1998; Tanaka and North, 1993). 5-HT2A and 5-HT1A receptors are coexpressed by a large population of PFC neurons (Amargos-Bosch et al, 2004) and opposing effects of the activation of both receptors by 5-HT on pyramidal cell activity have been reported (Amargos-Bosch et al, 2004; Araneda and Andrade, 1991; Ashby et al, 1994). The 5-HT1A antagonist WAY-100635 previously has been found to block the increase in the reinforcement rate induced by a 10 mg/kg dose of fluoxetine (Cousins and Seiden, 2000). However, these same doses of WAY-100635 also produced a substantial enhancement of the response-rate decreasing effect of the 10 mg/kg fluoxetine dose. Nonetheless, it is possible that the administration of M100907 resulted in an enhanced 5-HT1A receptor-mediated transmission in PFC. However, additional 5-HT receptors may contribute to the apparent functional antagonism of 5-HT2A receptor-mediated effects that can be seen from electrophysiological studies both from in vivo preparations and prefrontal cortical slice preparations (Aghajanian and Marek, 1997, 1999; Lakoski and Aghajanian, 1985; Marek, 2000).
A recent review has discussed a number of double-blind, placebo-controlled studies which together suggest that a combination of drugs which block both the 5-HT2 family of receptors and SERT would have greater antidepressant efficacy than SSRIs alone (Marek et al, 2003). The initial report on the olanzapine–fluoxetine combination in treatment-resistant, nonpsychotic unipolar depression found that within 1 week of adding on 5 mg/day of olanzapine onto ongoing fluoxetine treatment, patients had a superior response to those patients having placebo added on to ongoing fluoxetine treatment (Shelton et al, 2001). The superior efficacy of the olanzapine–fluoxetine combination in bipolar I depression compared to olanzapine alone or placebo further supports the hypothesis that the blockade of a 5-HT2 receptor and SERT results in superior antidepressant efficacy than simpl blockade of SERT alone (Tohen et al, 2003) The major limitation in extrapolating to the critical receptor(s) underlying this boost in clinical efficacy is the rich pharmacology for mianserin, mirtazapine, and olanzapine. All three drugs would be expected to block the 5-HT2C receptor at exposures similar to those blocking 5-HT2A receptors. All three drugs are even more potent at the histamine H1 receptor than the 5-HT2 family of receptors. While mirtazapine and mianserin also potently block alpha-2 noradrenergic receptors, mirtazapine appears to have a wider profile of action on noradrenergic autoreceptors than does mianserin. Olanzapine appears to be more potent in blocking 5-HT2A receptors than dopamine D2 receptors from in vivo PET studies with human subjects (Kapur et al, 1999), in agreement with in vitro or ex vivo binding data with native rat or cell lines transfected with human receptors (Bymaster et al, 1996; Schotte et al, 1996).
Multiple lines of evidence are consistent with the hypothesis that blockade of 5-HT2A receptors might enhance the therapeutic effectiveness of SSRIs. First and foremost, a number of placebo controlled trials have found that addition of drugs, which share a common pharmacological action of 5-HT2 receptor blockade (eg, mianserin, mirtazapine and olanzapine), appear to enhance the antidepressant efficacy of SSRIs (Marek et al, 2003). Second, downregulation of 5-HT2A receptors is a common and reasonably specific characteristic for known antidepressant drugs (Peroutka and Snyder, 1980), although some controversy exists regarding the effects of SSRIs. Third, a trend exists for upregulation of 5-HT2A receptor binding in discrete prefrontal cortical regions of suicide victims from postmortem studies (Pandey et al, 2002; Stockmeier et al, 1997). Fourth, blockade of 5-HT2A receptors is one of the most common and potent shared pharmacological actions for a number of antidepressants (Marek et al, 1992) which do not appear to have antidepressant efficacy in patients due to blockade of SERT (serotonin transporters), NET (norepinephrine transporters), or monoamine oxidase (MAO; eg, mirtazapine, mianserin, nefazodone, trazodone, and iprindole). Fifth, intolerance to high doses of paroxetine in elderly patients due to difficulty with arousal, concentration, agitation, and sleep disturbances appears to be related to a single-nucleotide polymorphism (SNP) in the 5-HT2A receptor gene (Murphy et al, 2003). One cannot conclude whether this pharmacological effect reflects an enhancement of paroxetine-induced adverse events or a deterioration of a cluster of core depressive symptoms. Sixth, activation of 5-HT2A receptors appears to result predominantly in excitatory actions in the neocortex and prefrontal cortex in contrast to the widespread inhibitory actions of 5-HT itself (Aghajanian and Marek, 1997; Araneda and Andrade, 1991; Ashby et al, 1994; Tanaka and North, 1993).
In summary, the present results suggest that selective blockade of 5-HT2A receptors may complement the behavioral effects of SERT inhibition. These behavioral observations would appear consistent with the general opposing effects of 5-HT2A and many non-5-HT2A receptors throughout cortical-thalamic-striatal-amygdaloid circuits. One important implication of the present studies for clinical investigation is whether blockade of 5-HT2A receptors contributes to the enhancement of antidepressant effects of SSRIs found with mirtazapine, mianserin, olanzapine, and risperidone. Obviously, testing the combination of a highly selective 5-HT2A receptor antagonist like M100907 together with an SSRI or a new chemical entity with selective blockade of both 5-HT2A and SERT in the same molecule (Puller et al, 2000; Schmidt et al, 2001) would be a critical clinical experiment to test this hypothesis. A second implication open for future studies is whether selective blockade of 5-HT2A receptors can also have an additive or synergistic action in the treatment of other diverse neuropsychiatric syndromes for which SSRIs are a useful therapeutic modality (Marek et al, 2003).
References
Adell A, Artigas F (1998). A microdialysis study of the in vivo release of 5-HT in the median raphe nucleus of the rat. Br J Pharmacol 125: 1361–1367.
Aghajanian GK, Marek GJ (1997). Serotonin induces excitatory postsynaptic potentials in apical dendrites of neocortical pyramidal cells. Neuropharmacology 36: 589–599.
Aghajanian GK, Marek GJ (1999). Serotonin, via 5-HT2A receptors, increases EPSCs in layer V pyramidal cells of prefrontal cortex by an asynchronous mode of glutamate release. Brain Res 825: 161–171.
Amargos-Bosch M, Bortolozzi A, Puig MV, Serrats J, Adell A, Celada P et al (2004). Co-expression and in vivo interaction of serotonin1a and serotonin2a receptors in pyramidal neurons of prefrontal cortex. Cereb Cortex 14: 281–299.
Araneda R, Andrade R (1991). 5-Hydroxytryptamine2 and 5-Hydroxytryptamine1A receptors mediate opposing responses on membrane excitability in rat association cortex. Neuroscience 40: 399–412.
Ashby CR, Edwards E, Wang RY (1994). Electrophysiological evidence for a functional interaction between 5-HT1A and 5-HT2A receptors in the rat medial prefrontal cortex: an iontophoretic study. Synapse 17: 173–181.
Borsini F (1995). Role of the serotonergic system in the forced swimming test. Neurosci Biobehav Rev 19: 377–395.
Bymaster FP, Calligaro DO, Falcone JF, Marsh RD, Moore NA, Tye NC et al (1996). Radioceptor binding profile of the atypical antipsychotic olazepine. Neuropsychopharmacology 14: 87–96.
Cousins MS, Seiden LS (2000). The serotonin-1A receptor antagonist WAY-100635 modifies fluoxetine's antidepressant-like profile on the differential reinforcement of low rates 72-s schedule in rats. Psychopharmacology 148: 438–442.
Delgado PL, Charney DS, Price LH, Aghajanian GK, Landis H, Heninger GR (1990). Serotonin function and the mechanism of antidepressant action. Reversal of antidepressant-induced remission by rapid depletion of plasma tryptophan. Arch Gen Psychiatry 47: 411–418.
Delgado PL, Miller HL, Salomon RM, Licinio J, Krystal JH, Moreno FA et al (1999). Tryptophan-depletion challenge in depressed patients treated with desipramine or fluoxetine: implications for the role of serotonin in the mechanism of antidepressant action. Biol Psychiatry 46: 212–220.
Hervas I, Artigas F (1998). Effect of fluoxetine on extracellular 5-hydroxytryptamine in rat brain. Role of autoreceptors. Eur J Pharmacol 358: 9–18.
Hirose S, Ashby CRJ (2002). An open pilot study combining risperidone and a selective serotonin reuptake inhibitor as initial antidepressant therapy. J Clin Psychiatry 63: 733–736.
Jakab RL, Goldman-Rakic PS (1998). 5-HT2A serotonin receptors in the primate cerebral cortex: possible site of action of hallucinogens in pyramidal cell apical dendrites. Proc Natl Acad Sci USA 95: 735–740.
Jakab RL, Goldman-Rakic PS (2000). Segregation of serotonin 5-HT2A and 5-HT3 receptors in inhibitory circuits of the primate cerebral cortex. J Comp Neurol 417: 337–348.
Kapur S, Zipursky RB, Remington G (1999). Clinical and theoretical implications of 5-HT2 and D2 receptor occupancy of clozapine, risperidone, and olanzapine in schizophrenia. Am J Psychiatry 156: 286–293.
Kehne JH, Baron BM, Carr AA, Chaney SF, Elands J, Feldman DJ et al (1996). Preclinical characterization of the potential of the putative atypical antipsychotic MDL 100,907 as a potent 5-HT2A antagonist with a favorable CNS safety profile. J Pharmacol Exp Ther 277: 968–981.
Lakoski JM, Aghajanian GK (1985). Effects of ketanserin on neuronal responses to serotonin in the prefrontal cortex, lateral geniculate and dorsal raphe nucleus. Neuropharmacology 24: 265–273.
Luttinger D, Freedman M, Hamel L, Ward SJ, Perrone M (1985). The effects of serotonin antagonists in a behavioral despair procedure in mice. Eur J Pharmacol 107: 53–58.
Marcoli M, Maura G, Munari C, Ruelle A, Raiteri M (1999). Pharmacological diversity between native human 5-HT1B and 5-HT1D receptors sited on different neurons and involved in different functions. Br J Pharmacol 126: 607–612.
Marek GJ (2000). A novel approach to the identification of psychiatric drugs: serotonin–glutamate interactions in the prefrontal cortex. CNS Drug Rev 6: 205–217.
Marek GJ, Carpenter LL, McDougle CJ, Price LH (2003). Synergistic action of 5-HT2A antagonists and selective serotonin reuptake inhibitors in neuropsychiatric disorders. Neuropsychopharmacology 28: 402–412.
Marek GJ, Li AA, Seiden LS (1989). Selective 5-hydroxytryptamine2 antagonists have antidepressant-like effects on differential-reinforcement-of-low-rate 72-second schedule. J Pharmacol Exp Ther 250: 52–59.
Marek GJ, McDougle CJ, Price LH, Seiden LS (1992). A comparison of trazodone and fluoxetine: implications for a serotonergic mechanism of antidepressant action. Psychopharmacology 109: 2–11.
Marek GJ, Seiden LS (1988). Effects of selective 5-hydroxytryptamine-2 and nonselective 5-hydroxytryptamine antagonists on the differential-reinforcement-of-low-rate 72-second schedule. J Pharmacol Exp Ther 244: 650–658.
Marek GJ, Seiden LS (1994). Antidepressant drug screens and the serotonin system. In: Palomo T, Archer T (eds). Strategies for Studying Brain Disorders: Depressive, Anxiety and Drug Abuse Disorders. Vol 1. Farrand Press: London. pp 23–40.
Marek GJ, Wright RA, Gewirtz JC, Schoepp DD (2001). A major role for thalamocortical afferents in serotonergic hallucinogen receptor function in neocortex. Neuroscience 105: 113–126.
Martin JR, Bos M, Jenck F, Moreau J, Mutel V, Sleight AJ et al (1998). 5-HT2C receptor agonists: pharmacological characteristics and therapeutic potential. J Pharmacol Exp Ther 286: 913–924.
Maura G, Marcoli M, Tortarolo M, Andrioli GC, Raiteri M (1998). Glutamate release in human cerebral cortex and its modulation by 5-hydroxytryptamine acting at h 5HT1D receptors. Br J Pharmacol 123: 45–50.
Miner LAH, Backstrom JR, Sanders-Bush E, Sesack SR (2003). Ultrastructural localization of serotonin2A receptors in the middle layers of the rat prelimbic prefrontal cortex. Neuroscience 116: 107–117.
Murphy GMJ, Kremer C, Rodriques HE, Schatzberg AF (2003). Pharmacogenetics of antidepressant medication intolerance. Am J Psychiatry 160: 1830–1835.
O'Connor M, Silver H (1998). Adding risperidone to selective serotonin reuptake inhibitor improves chronic depression. J Clin Psychopharmacol 18: 89–90.
O'Donnell JM, Marek GJ, Seiden LS (2005). Antidepressant effects assessed using behavior maintained under a differential-reinforcement-of-low-rate (DRL) operant schedule. Neurosci Biobehav Rev (in press).
O'Donnell JM, Seiden LS (1982). Effects of monoamine oxidase inhibitors on performance during differential reinforcement of low response rate. Psychopharmacology 78: 214–218.
Ostroff RB, Nelson JC (1999). Risperidone augmentation of SSRIs in major depression. J Clin Psychiatry 60: 256–259.
Pandey GN, Dwivedi Y, Rizavi HS, Ren X, Pandey SC, Pesold C et al (2002). Higher expression of 5-HT2A receptors in the postmortem brains of teenage suicide victims. Am J Psychiatry 159: 419–429.
Paxinos G, Watson C (1986). The Rat Brain in Stereotoxic Coordinates. Academic Press: Orlando, FL.
Pericic D (2003). Swim stress inhibits 5-HT2A receptor-mediated head twitch behavior in mice. Psychopharmacology 167: 373–379.
Peroutka SJ, Snyder SH (1980). Long-term antidepressant treatment decreases spiroperidol-labeled serotonin receptor binding. Science 210: 88–90.
Puig MV, Celada P, Diaz-Mataix L, Artigas F (2003). In vivo modulation of the activity of pyramidal neurons in the rat medial prefrontal cortex by 5-HT2A receptors. Relationship to thalamocortical afferents. Cereb Cortex 13: 870–882.
Puller IA, Carney SL, Colvin EM, Lucaites VL, Nelson DL, Wedley S (2000). LY367265, an inhibitor of the 5-hydroxytryptamine transporter and 5-hydroxytryptamine 2A receptor antagonist: a comparison with the antidepressant, nefazodone. Eur J Pharmacol 407: 39–46.
Redrobe JP, Bourin M (1997). Partial role of 5-HT2 and 5-HT3 receptors in the activity of antidepressants in the mouse forced swimming test. Eur J Pharmacol 325: 129–135.
Richards JB, Seiden LS (1991). A quantitative interresponse time analysis of DRL performance differentiates similar effects of the antidepressant desipramine and the novel anxiolytic gepirone. J Exp Anal Behav 56: 173–192.
Schmidt CJ, Fox CB, Harms JF, Wylie P, Seegar TF, Guanowsky V et al (2001). CP-646,781: a potent dual SSRI/5-HT2A receptor agonist. Socr Neurosci Abstr 27: Program no. 665-17.
Schotte A, Janssen PFM, Gommeren W, Luyten WH, Van Gompel P, Lesage AS et al (1996). Risperidone compared with new and reference antipsychotic drugs: in vitro and in vivo receptor binding. Psychopharmacology 124: 57–73.
Schreiber R, Brocco M, Audinot V, Gobert A, Veiga S, Millan MJ (1995). 1-(2,5-Dimethoxy-4 iodophenyl)-2-aminopropane)-induced head-twitches in the rat are mediated by 5-hydroxytryptamine(5-HT)2A receptors: modulation by novel 5-HT2A/2C antagonists, D1 antagonists and 5-HT1A agonists. J Pharmacol Exp Ther 273: 101–112.
Seiden LS, Dahms JL, Shaughnessy RA (1985). Behavioral screen for antidepressants: the effects of drugs and electroconvulsive shock on performance under a differential-reinforcement-of-low-rate schedule. Psychopharmacology 86: 55–60.
Shelton RC, Tollefson GD, Tohen M, Stahl S, Gannon KS, Jacobs TG et al (2001). A novel augmentation strategy for treating resistant major depression. Am J Psychiatry 158: 131–134.
Sokolowski JD, Seiden LS (1999). The behavioral effects of sertraline, fluoxetine, and paroxetine differ on the differential-reinforcement-of-low-rate 72-second operant schedule in the rat. Psychopharmacology 147: 153–161.
Stockmeier CA, Dilley GE, Shapiro LA, Overholser JC, Thompson PA, Meltzer HY (1997). Serotonin receptors in suicide victims with major depression. Neuropsychopharmacology 16: 162–173.
Tanaka E, North RA (1993). Actions of 5-hydroxytryptamine on neurons of the rat cingulate cortex. J Neurophysiol 69: 1749–1757.
Tohen M, Vieta E, Calabrese J, Ketter TA, Sachs G, Bowden C et al (2003). Efficacy of olanzapine and olanzapine–fluoxetine combination in the treatment of bipolar I depression. Arch Gen Psychiatry 60: 1079–1088.
Willins DL, Deutch AY, Roth BL (1997). Serotonin 5-HT2A receptors are expressed on pyramidal cells and interneurons in the rat cortex. Synapse 27: 79–82.
Zhang W, Perry KW, Wong DT, Potts BD, Bao J, Tollefson GD et al (2000). Synergistic effects of olanzapine and other antipsychotic agents in combination with fluoxetine on norepinephrine and dopamine release in rat prefrontal cortex. Neuropsychopharmacology 23: 250–262.
Zhou F-M, Hablitz JJ (1999). Activation of serotonin receptors modulates synaptic transmission in rat cerebral cortex. J Neurophysiol 82: 2989–2999.
Acknowledgements
This work was previously presented at the 2001 Society for Neuroscience meeting (San Diego, CA) and the 2001 meeting of the American College of Neuropsychopharmacology (San Juan, Puerto Rico). This study was supported by PHS Grants K08 MH01551, R01 MH62186, a NARSAD Young Investigator Award (1999 Fairfax Investigator Award), the state of Connecticut (GJM), and National Institutes of Health Grants FIS 01/1147 and SAF2001-2133 (FA) We appreciate Dr Younglim Lee's review of the manuscript. We thank Nigel Henry, Sara Heron, Andrew Kwak, Megan Lennon, Boting Zhang, and Leticia Campa for technical assistance. We also thank Leslie Rosello for secretarial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Marek, G., Martin-Ruiz, R., Abo, A. et al. The Selective 5-HT2A Receptor Antagonist M100907 Enhances Antidepressant-Like Behavioral Effects of the SSRI Fluoxetine. Neuropsychopharmacol 30, 2205–2215 (2005). https://doi.org/10.1038/sj.npp.1300762
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1300762
Keywords
This article is cited by
-
5-HT 2A and 5-HT 2C receptor antagonism differentially modulate reinforcement learning and cognitive flexibility: behavioural and computational evidence
Psychopharmacology (2024)
-
Effect of psilocybin on marble burying in ICR mice: role of 5-HT1A receptors and implications for the treatment of obsessive-compulsive disorder
Translational Psychiatry (2023)
-
High-throughput brain activity mapping and machine learning as a foundation for systems neuropharmacology
Nature Communications (2018)
-
Premature responses in the five-choice serial reaction time task reflect rodents’ temporal strategies: evidence from no-light and pharmacological challenges
Psychopharmacology (2016)
-
Increased Serotonin Transporter Expression Reduces Fear and Recruitment of Parvalbumin Interneurons of the Amygdala
Neuropsychopharmacology (2015)