Abstract
Objective: We applied paired transcranial magnetic stimulation (pTMS) to patients with post-traumatic stress disorder (PTSD) secondary to minor accidental head trauma. Our purpose was to determine the potential abnormality of motor cortex excitability in this pathologic condition.
Methods: pTMS stimulation, according to the conditioning–test paradigm employing interstimulus intervals (ISIs) of 1–6 ms, was used to investigate intracortical inhibition in control subjects and patients with PTSD. The study population consisted of 14 patients who had developed PTSD following minor head trauma, 12 healthy volunteers without a clinical history of head trauma and 11 healthy subjects who had reported accidental minor head trauma 1–4 months before the study. This clinical electrophysiologic study was performed at the Department of Neuroscience, University of Rome “Tor Vergata.”
Results: All patients with PTSD exhibited a significantly lower motor evoked potential (MEP) inhibition than controls at 2 ms, 3 ms and 4 ms ISI. The statistical analysis of the pTMS protocol showed a significant effect ( F2,36 = 25.63, p < 0.001) of the factor “group,” because patients with PTSD showed a mean conditioned MEP amplitude higher than that observed in both control groups for all 6 ISIs analyzed. The “ISI” factor was also significant ( F5,180 = 89.85, Greenhouse–Geisser ɛ = 0.35; p < 0.001), with the mean conditioned MEP amplitude increasing from 22.5% to 127.8% as the ISI increased from 1 ms to 6 ms. Finally, the interaction of group with ISI was also significant ( F10,180 = 8.97, p < 0.001), showing that the condition of PTSD secondary to head trauma was able to affect the MEP amplitude at different ISIs.
Conclusions: Our results demonstrate that PTSD can give rise to abnormalities in intracortical inhibition. Our results provide further evidence that alterations in cortical inhibitory circuits may underlie specific forms of neuroticism in humans.
Introduction
Aggression or motor vehicle accidents, especially when associated with minor head trauma, are among the most frequent causes of post-traumatic stress disorder (PTSD). PTSD is a condition in which individuals re-experience phenomena and have avoidance behaviours and somatic disturbances coupled with sleep disorders and, typically, hyperarousal. Exclusion of other mental or organic disorders and the presence of symptoms that last for at least 1 month are essential requirements for the diagnosis of PTSD according to the criteria of the Diagnostic and Statistical Manual of Mental Disorders, fourth edition (DSM-IV).1
Although the results of functional neuroimaging studies and the hyperarousal typical of this disorder strongly suggest that abnormal brain excitability may play a key role in the genesis of PTSD symptoms,2–5 a neurophysiologic study aimed at addressing this critical aspect of the disorder is still lacking.
Transcranial magnetic stimulation (TMS) has proved to be capable of evaluating motor cortex excitability by measuring the threshold of motor evoked potentials (MEPs) and intracortical inhibition by ad hoc paired-pulse paradigms.6,7 The application of this technique has substantially contributed to clarification of the pathophysiologic mechanisms underlying other neuropsychiatric conditions, by revealing changes in excitability of the corticospinal tracts.7,8 These changes are generally ascribed to an imbalance between glutamate (the main excitatory neurotransmitter) and the inhibitory transmitter γ-aminobutyric acid (GABA) within the cortex.9–12 In this respect, stress-induced long-term potentiation of glutamate-mediated transmission might represent a synaptic correlate of the maintenance of traumatic memories that cause PTSD, and a number of studies have shown that PTSD is associated with long-term changes in brain structures and systems that mediate memory and the stress response.13,14 It is, therefore, conceivable that long-lasting alterations of cortical excitability may underlie, at least in part, some of the mental symptoms of PTSD that follow a minor head injury.
In the present study, we applied TMS in an attempt to investigate whether changes in cortical excitability are associated with the development of PTSD disorder after accidental head trauma. In particular, paired stimulation, with different interstimulus intervals (ISIs), was applied in order to gain insights into the functioning of intracortical inhibitory transmission in this pathologic condition.6
Methods
Fourteen patients with PTSD secondary to head trauma (8 women and 6 men, aged between 18 and 47 yr) underwent neurophysiologic examination with TMS at 1–6 months after the trauma. The clinical diagnosis of PTSD was derived according to DSM-IV criteria.
Before TMS investigation, subjects underwent a complete neurologic examination, standard electroencephalography, and brain computed tomography or magnetic resonance imaging (MRI). In addition, they underwent the Minnesota Multiphasic Personality Inventory (MMPI)15 examination and the State–Trait Anxiety Inventory16 (STAI)-based evaluation for anxiety. Eligible patients were considered to be those without brain injury (no loss of consciousness, Glasgow Coma Scale score 15) and normal findings on brain computed tomography or MRI. Patients were excluded from the study if they had a clinical history of epilepsy or neurologic deficits and conditions that could affect nerve conduction along the spinal cord (concomitant cervical injury, treatment with neurotropic drugs, neuropathy with conduction block). Patients were excluded if they had other primary major psychiatric illnesses such as major depressive disorders, obsessive–compulsive disorders, panic disorders, or comorbid disorders including alcohol abuse or dependence, schizophrenia or bipolar disorders.
Patients’ neurophysiologic data were age-matched against those of a control population represented by 12 healthy volunteers (7 women and 5 men) who, analogous to the patients, were not familiar with the technique of TMS. We also studied 11 subjects (5 women and 6 men) who reported a minor head trauma 1–4 months before the study but did not develop PTSD or other neurologic or psychiatric sequelae. Anxiety and obsessive–compulsive disorder have been found to be associated with increased motor cortex excitability.7,8 Control subjects, therefore, underwent a complete psychiatric examination with the MMPI and the STAI scale, and subjects who exhibited traits of obsessive–compulsive disorder or anxiety (score > 35 either on the STAI State Anxiety Form or the Trait Anxiety Form) were not included.
Patients and controls were statistically comparable for age (patients: 36.4 [and standard deviation {SD} 8.4] yr, controls without trauma: 38.4 [SD 6.2] yr, controls with trauma: 39 [SD 9.3] yr) and time interval since head trauma (patients: 2.1 [SD 1.4] mo, controls with trauma: 2.4 [SD 1.6] mo). None of the control subjects or patients were being treated with neurotropic drugs. Informed consent for the procedures used was obtained from the whole examined population, and the Ethics Committee of the University of Rome “Tor Vergata” approved the study.
Recording and stimulating procedures
Seizure disorder can be a sequela of all degrees of head trauma.17 Therefore, to limit any risk of inducing seizures by the use of repetitive TMS, in the present study we chose to concentrate on the GABA-mediated intracortical inhibition profile by using a paired TMS (pTMS) technique with ISIs ranging from 1 ms to 6 ms.18 The TMS examination, which was performed with the subject comfortably reclined on a bed in a quiet room, lasted on average 40 minutes. MEPs were recorded with surface electrodes in thenar muscles, during complete muscle relaxation and with open eyes.19 The active electrode was placed over the motor point with the reference on the metacarpophalangeal joint. An acoustic feedback monitored the electromyographic background activity in order to detect and avoid interference possibly induced by voluntary movements; contaminated trials were discarded. A time window of 50 ms preceding stimulation was visualized online in order to monitor the level of muscle relaxation. Recordings were acquired with a filtering bandwidth of 20–2000 Hz and a sampling rate of 10 kHz and were stored for offline analysis.
We used pTMS, according to the conditioning–test paradigm employing short ISIs, to investigate the time course of intracortical excitability.6 This was achieved by using a figure of 8 coil, which was 14 cm in transversal diameter, connected to 2 Magstim 200 stimulators through a Bi-stim module (Magstim, Dyfield, UK). Pairs of stimuli were discharged, each having different intensities, with conditioning pulses delivered from 1 ms to 6 ms before test stimulation. The coil was held manually in an anteroposterior direction, with the handle pointing backward at about 45° toward the occipital pole. The centre of the coil was placed over the left central sulcus, on the scalp region corresponding to the hand motor area, so as to activate pyramidal neurons transsynaptically. The site where MEPs with the lowest intensity were elicited in the contralateral relaxed target muscle was located at around 5–6 cm lateral to Cz along the earlobe line and was marked with a pencil in order to ensure the same coil position during the whole TMS examination. The resting MEP threshold was determined to be the minimum TMS intensity required to produce MEPs greater than or equivalent to 50 μV on 5 or more consecutive trials of stimulation delivered at least 5 s apart. After this, the active MEP threshold was determined according to the same criteria but in the presence of a voluntary contraction (40% of maximum, as determined via a home-made manual transducer), which was monitored with visual and auditory feedback.
pTMS testing was performed as follows: the conditioning pulse intensity was set at 10% below the active MEP threshold. This intensity was chosen to ensure that this pulse would not evoke any physiologically significant activity in the corticospinal tract. The test pulse intensity was set at a level that produced an MEP of about 500 μV, as originally designed. 6,20 The ISIs tested were 1 ms, 2 ms, 3 ms, 4 ms, 5 ms and 6 ms and were chosen to sample conditioned MEP amplitude during the inhibited phase of the conditioning effect. Ten trials were delivered at each ISI with isolated test pulses interspersed on every fifth trial. The order of the ISIs was varied randomly. The mean intertrial interval was 7 s and was also varied randomly.7
Neurophysiologic data analysis
The following neurophysiologic parameters were analyzed: (1) the value of the resting motor threshold for test stimuli and the active motor threshold for conditioning ones, expressed as a percentage of the stimulator maximal output; (2) the amplitudes of test and conditioned MEPs measured from peak to peak (negativity upward); (3) MEP mean amplitudes calculated separately for each ISI (from 1 ms to 6 ms) and the differences in amplitude between test and conditioned MEPs, expressed as a percentage of test stimulus alone.
Statistical analysis
Differences in MEP excitability thresholds were evaluated with the Mann–Whitney test. Statistical significance was assumed for values of p < 0.05.
MEP amplitude changes obtained in response to pTMS were expressed as a percentage of MEP control size, that is, resulting from test stimulus alone, in both patients and controls. The statistical evaluation of pTMS data included a 2-way analysis of variance (ANOVA) corrected by the Greenhouse–Geisser method when more than 2 levels were present in a “within” factor. Thus, the electrophysiologic data obtained in the 3 groups studied were analyzed together by means of a between factor “group” with 3 levels (patients with PTSD v. controls without trauma v. controls with trauma) and a within factor “ISI,” with 6 levels, corresponding to the ISI sequence investigated. Whenever a significant interaction between factors was found, the single differences were assessed by means of the post hoc Tukey Honestly Significant Difference (HSD) test. Significance was set at p < 0.05.
An additional evaluation with a 2-way ANOVA was conducted comparing the patients with anxiety (n = 6; 3 women, 3 men; mean age 30.5 [SD 7.2] yr; mean time interval since trauma 2.6 [SD 0.8] mo; score on the STAI State Anxiety Form > 45) and the patients who did not report anxiety (n = 8; 5 women, 3 men; mean age 38.9 [SD 8.3] yr; mean time interval since trauma 1.8 [SD 0.5] mo; score on the STAI State Anxiety Form < 45) because of the possible influence that this symptom can induce on the profile of intracortical inhibition.7
Results
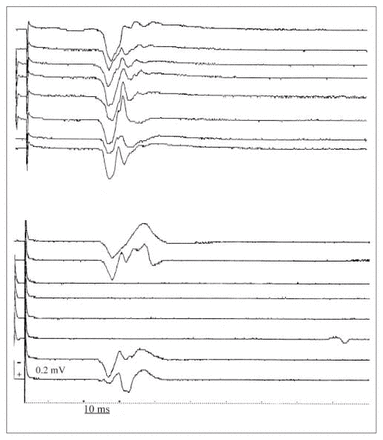
Anxiety was found at STAI evaluation in 6 patients with PTSD. No difference in both resting (TMS intensity for test stimulation) and active (TMS intensity for conditioning stimulation during target muscle contraction) motor thresholds was found between patients and the 2 control groups (test: 72.6% [SD 9.4%] v. 73.4% [SD 6.9%] v. 72.9% [SD 8.2%]; conditioning: 42.5% [SD 7.2%] v. 44.7% [SD 6.2%] v. 43.6% [SD 9.1%] for patients with PTSD, controls without trauma, controls with trauma, respectively). Unconditioned MEPs had similar average amplitudes in the groups under investigation (controls without trauma: 497 [SD 80] μV, controls with trauma: 516 [SD 90] μV, patients with PTSD: 550 [SD 140] μV) (example shown in Fig. 1). In addition, no significant change in MEP threshold was observed when anxious patients with PTSD were compared statistically with those patients who did not exhibit anxiety. These data are in line with a previous report in which anxiety has been reported to correlate with abnormal paired-pulse responses but not with altered MEP threshold.7
Right-hand motor evoked potentials (MEPs) from a patient with post-traumatic stress disorder (PTSD) (upper panel) and a control subject (lower panel). In each panel, the sequence of traces displays the same rule of recording: the upper and lower pairs of traces are evoked in response to the test stimulus alone, whereas traces in the middle are the result of paired (conditioning and test) stimulation, with an interstimulus interval of 3 ms. Note the absence of the physiologic MEP suppression in the patient with PTSD compared with the control subject.
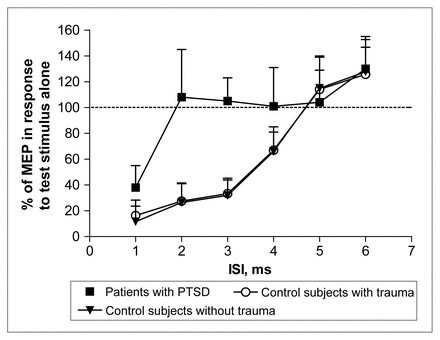
A significant loss of MEP inhibition, normally produced by pTMS at first ISI,6 was found in all patients with PTSD in comparison with both control groups at 2 ms, 3 ms and 4 ms ISI (Fig. 1, Fig. 2). In fact, the statistical analysis of pTMS data showed a significant effect (F2,36 = 25.63, p < 0.001) of the factor “group,” because in patients with PTSD the mean conditioned MEP amplitude over the 6 ISI was higher (98.87%) than that observed in the other 2 populations (63.19% and 64.11% for controls without trauma and controls with trauma, respectively). The ISI factor was also significant (F5,180 = 89.85, Greenhouse–Geisser ɛ = 0.35; p < 0.001), as the mean “conditioned” MEP amplitude increased from 22.5% to 127.8% as the ISI increased from 1 ms to 6 ms. Finally, the group × ISI interaction was also significant (F10,180 = 8.97, p < 0.001), showing that the effect of the conditioning stimulus was different in the 3 studied groups at different ISI. In fact, the Tukey HSD test illustrated a significant loss of MEP inhibition at 2 ms, 3 ms and 4 ms ISI in patients with PTSD in comparison with both controls without trauma (2 ms: p < 0.001, 3 ms: p < 0.001 and 4 ms: p < 0.01) and controls with trauma (2 ms: p < 0.001, 3 ms: p < 0.001 and 4 ms: p < 0.05). It is noticeable that no statistical difference was found between the 2 control groups (Fig. 2).
Average time course of intracortical inhibition in 12 control subjects without trauma, 11 control subjects with trauma and 14 patients with PTSD. At each interstimulus interval (ISI), the size of the conditioned MEP is expressed as a percentage of the size of the MEP in response to the test stimulus alone. Note the large difference between the curves, indicating the lack of inhibition in patients with PTSD, particularly from 2 ms to 4 ms of ISIs. The results are given here as means (and standard deviation).
Discussion
In the present study, we provided evidence that PTSD, when following minor head trauma, is coupled with the loss of physiologic inhibition of cortical stimulation during pTMS. The evidence that subjects who had experienced trauma to the head but no PTSD did not exhibit abnormal intracortical inhibition suggests that the lack of intracortical inhibition is strictly correlated with the presence of PTSD symptoms rather than with the head trauma itself.
The excitability of corticospinal neurons, the activation of which is responsible for motor evoked responses, is finely regulated by both excitatory and inhibitory inputs.21 Although it is generally accepted that MEPs mainly originate from the stimulation of excitatory axons impinging on corticospinal neurons,20,22 the physiologic role of GABAergic inputs in the modulation of cortical excitability can be evaluated by paired-pulse stimulation with short ISIs.6,9,10,18,21,23 Interestingly, GABA-mediated inhibition of cortical pyramidal neurons is essentially intrinsic, arising from local interneurons responsible for a delayed inhibition of corticospinal neurons during TMS. In accordance with this, whereas the amplitude and threshold of motor responses evoked from a single pulse are unaffected by pharmacologic agents that enhance GABA-mediated transmission, these compounds increase MEP inhibition during pTMS.9 The evidence that pTMS-mediated MEP inhibition occurs even when the first, conditioning stimulus is unable to produce an MEP strongly suggests that cortical GABAergic interneurons are particularly prone to excitation.
Our data, therefore, suggest that durable functional and/or structural injury of these highly excitable interneurons can account for the impairment of cortical inhibition after traumatic events and, possibly, for the clinical symptoms of PTSD. In this respect, several neuroimaging findings suggest that after psychological trauma, biologic changes are not restricted to dysregulation of neurochemical systems but also involve alterations in brain function and structure. In particular, a number of structural MRI studies have shown that subjects with PTSD have a hippocampal volume that is smaller than normal,24–29 although other groups have failed to show reduced hippocampal volume in PTSD.30–35 Brain structures other than the hippocampus have received less attention, although a few studies have reported whole-brain volume reduction, 30 reduced total white-matter volume,28 smaller corpus callosum,30 larger superior temporal gyrus grey-matter volume36 and reduction in anterior cingulate grey-matter volume. 37 On the other hand, functional neuroimaging has revealed greater activation of the amygdala, anterior paralimbic structures and, importantly, Broca’s region and other neocortical regions in response to trauma-related stimuli in individuals with PTSD.38–40 Furthermore, a decrease in N-acetyl-aspartate, an indicator of neuronal integrity, has been found by means of proton magnetic resonance spectroscopy in the hippocampus of patients with PTSD.34,41
In the patients with PTSD included in this study, the observed impairment of GABA-mediated MEP inhibition may also reflect a selective vulnerability of cortical GABAergic interneurons to glutamate-mediated excitotoxic events. Accordingly, a significant increase in glutamate concentration occurs transiently in the brain following head trauma,42,43 an effect paralleled by increased sensitivity of cortical neurons to glutamate receptor stimulation.43 It is, therefore, conceivable that the combination of the 2 events may favour excitotoxic events in highly excitable neurons, thereby causing a preferential injury of GABA interneurons.
Our findings are in line with basic experimental data indicating that acute stress affects brain activity and promotes long-term changes of synaptic efficacy. In this respect, long-term potentiation of excitatory synapses is the most extensively accepted form of neuroplasticity, and it is believed to be the substrate for both explicit and implicit learning and memory processes. Interestingly, this form of synaptic plasticity follows massive stimulation of glutamate receptors44,45 and is primed by environmental physical and mental stressful events.46–49 It can be postulated, therefore, that similar plastic reorganization changes take place in patients who develop PTSD, accounting for the neurophysiologic abnormalities found in our study. According to this hypothesis, it has been reported that slow (< 1 Hz) repetitive TMS, a procedure believed to induce long-term depression of synaptic transmission or depotentiation of pathologic synaptic potentiation,50 exerts beneficial effects in patients with PTSD.51,52
The evaluation of excitatory ISIs, obtained with longer intervals, 9,53 in addition to the inhibitory ones, could also have been informative regarding the dysregulation of excitatory/inhibitory mechanisms at cortical levels. However, to limit any possible seizures induced by cortical stimulation, we decided to select a procedure that should be reasonably short and at the same time eloquent.
Taken together with the recent findings that motor cortex excitability correlates with obsessive–compulsive disorder and an anxiety-related personality trait,7 our data on PTSD support the conclusion that cortical hyperexcitability potentially underlies several psychiatric disturbances. Understanding the neurophysiologic bases of psychiatric disorders is essential for the development of more effective therapeutic strategies.
Footnotes
Medical subject headings: cortical excitability; hyperarousal; stress disorders, post-traumatic; transcranial magnetic stimulation.
Competing interests: None declared.
- Received April 2, 2003.
- Revision received December 11, 2003.
- Revision received May 1, 2004.
- Accepted May 18, 2004.