Are addictions diseases? Certainly they are included in recent and forthcoming versions of the DSM and other widely used diagnostic schemas. Still, the concept does not have universal support. Particularly widespread is the suspicion that drug use is a choice, even for individuals with long-time substance dependence.1,2 The idea cannot be completely dismissed. Most people who meet criteria for an addiction are eventually able to quit, and many accomplish this without the benefits of a clinical intervention.3–5 Among those who do receive treatment, a few words at the right moment from the right person can sometimes be as effective as a more extensive regimen.6 However, these features are primarily seen in mildly affected individuals.6 Even more essential to the issue, calling something a choice is not an explanation — it is the question. Why did the person make that choice? Why is stopping so difficult? And why is relapse so common even after withdrawal symptoms have dissipated?
Are addictions diseases, then?7 My Oxford English Dictionary (OED) describes illness and disease as the absence of ease and the presence of unpleasantness. Stedman’s Medical Dictionary definition demands more. Disease is a “morbid entity characterized usually by two or more of the following criteria: recognized etiologic agent(s), identifiable group of signs and symptoms, or consistent anatomical alterations.” The OED definition of disease is clearly met, as is at least 1 of Stedman’s 3 criteria (“signs and symptoms”). For example, addictions are associated with pervasive medical, emotional, personal and professional problems,8 and substance use disorders are among the top 10 causes of disability-adjusted life years lost worldwide.9–11
Do addictions also meet Stedman’s 2 other criteria? As a start, there is evidence of pre-existing vulnerability traits. Only a minority of people who try drugs and alcohol become addicted.12 Family,13 twin14–16 and adoption studies17,18 suggest that this differential risk comes 50% from genetic factors and 50% from environmental ones.19 Genome-wide association studies have tentatively identified specific contributions that are modest but replicable.20–22 Studies of gene × environment interactions suggest that the 2 variables augment the influence of the other.17,18
This differential vulnerability to addictions does not seem to reflect a unitary trait. Instead vulnerability arises along multiple trajectories with distinguishable temperamental features.23–25 Most are related to externalizing behaviours (e.g., impulsivity, sensation seeking, conduct disorders); others are related to internalizing ones (e.g., anxious-depressed mood).18,26–28 Some of the trajectories’ influences are substance-specific,29 potentially reflecting drug availability, sociocultural contexts30 and variations in genes that, for example, encode for the metabolism of ethanol31 and nicotine.32 Other influences are more general, including nonspecific genetic factors;14,15,33 family functioning; and prenatal, early life and adult stressors.17,18,34 Some trajectories share environmental factor overlap with 1 set of disease clusters and genetic overlap with another.29 The influence of these factors can be larger or smaller at different stages of the lifespan.30,35 Not surprisingly, there is substantial and varied comorbidity. Finally, once drug use itself begins, the neurochemical effects can be remarkably enduring. Repeated drug exposure can lead to long-lasting neuroplastic changes36,37 that alter responses to drugs and drug-related cues.38,39 Incentive processes become pathologically tied to a narrowed set of stimuli,39–41 and the neurocircuitry engaged expands from systems that influence voluntary reward-seeking behaviour to include those that regulate deeply ingrained, overlearned, difficult to alter stimulus-response habits.40–42 Among those with current addictions, disturbed striatal dopamine transmission and decreased cortical grey matter and function are among the best replicated findings in biological psychiatry.40,41
Based on these definitions, then, it is proposed that addictions should indeed be considered diseases. They are clinically relevant negative states (“signs and symptoms”) following from vulnerability traits that intersect with diverse factors (“etiologic agents”) to yield replicable neurobiological changes (“anatomical alterations”). They share characteristics with other medical diseases, yet have their own unique features. As with type II diabetes, hypertension and many cancers, there are genetic, biological and environmental influences. As with Tourette syndrome, patients can inhibit their compulsive behaviours, yet sustaining these choices is difficult and contextually modulated. Finally, in this view, an addiction is only 1 possible expression of the pre-existing traits. The exact expression varies with the trajectory and changes during development (e.g., shoplifting at age 10, substance abuse at age 15) and is modulated by life events, the presence or absence of particular cues and contexts and substance use itself (Fig. 1).
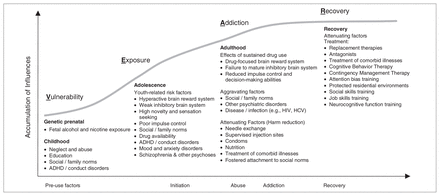
The VEAR model of addiction (Vulnerability, Exposure, Addiction, Recovery): transition points and treatment targets. The VEAR is based on SEIR models (Susceptibility, Exposure, Infection, Recovery) commonly used in epidemiology. The model highlights 3 points. First, addictions result from the influence of multiple factors along a trajectory. Second, there are multiple trajectories. Most addictions progress along trajectories characterized by i) externalizing behaviours, or ii) internalizing behaviours, with or without accompanying externalizing features. Third, each of the listed factors, including gene expression, can be influenced, providing multiple opportunities for intervention and treatment. Adapted with permission from Leyton and Cox.50 ADHD = attention-deficit/hyperactivity disorder; HCV = hepatitis C virus; HIV = human immunodeficiency virus.
These distinctive features of addiction as a disease are shared with other neuropsychiatric disorders,43–49 raising the possibility that addiction is not only a mental illness, but also a prototypical one. Although substance use disorders are unique in that disease expression (as an addiction) requires exposure to a drug, other psychiatric disorders also need external triggers. As with phobias, the abnormal response is tied to a specific set of stimuli. As with posttraumatic stress disorder, the precipitating agent is an exogenous event, exposure to which is thought to produce long-lasting effects on the brain that aggravate the underlying vulnerability. As with schizophrenia, it is thought to reflect a cumulative outcome of genetic, prenatal and early environmental psychosocial stressors. Indeed, converging evidence raises the possibility that nearly all major psychiatric illnesses are multifactorial, reflecting a gradient of neurodevelopmental processes and pleiotropic etiological trajectories.45
Identifying further the neurobiology associated with addictions and other mental illnesses will require more work and, more importantly, a change in research strategies. This includes gaining a better understanding of the basic neuro-science in both human and animal models and conducting large prospective follow-up studies to better characterize the relevant developmental changes. It will also require asking qualitatively different questions. Instead of testing whether people with diagnoses of disorder X have disturbances to neurobiological system X, we need to ask whether individual differences in a particular biological system are associated with cognitive–affective–behavioural phenomena of interest. This writer’s bet is that they do.
Acknowledgements
I thank Chawki Benkelfat and Robert O. Pihl for their feedback on an earlier version of this editorial and for many discussions over the years.