Abstract
Objective: To determine whether nitric oxide production levels differ in patients with deficit and nondeficit forms of schizophrenia.
Methods: We investigated plasma nitrate levels, an index of in vivo nitric oxide production, in patients with deficit syndrome (n = 11) and non-deficit syndrome (n = 14) and healthy controls (n = 12) with a combination of high-performance liquid chromatography and the Griess reaction.
Results: There was no difference found in mean plasma nitrite levels, but plasma nitrate levels of patients with deficit syndrome were significantly lower than those with non-deficit syndrome (28.0 [SEM 2.5] μmol/L v. 44.2 [SEM 5.5] μmol/L, p < 0.05).
Conclusions: A decline in nitric oxide production may be involved in primary negative symptoms in schizophrenia.
Introduction
Since being identified as an endothelium-derived relaxing factor, nitric oxide (NO), which is biosynthesized in neurons as well as endothelium from l-arginine (l-Arg) by nitric oxide synthase (NOS), has been focused on as a physiologically active substance.1 At the cellular level, NO can modulate hormone secretion in the neuroendocrine system,2 as well as the release and reuptake of monoaminergic neurotransmitters,3–7 and is also involved in the plasticity of neurons. In animal experiments, there is some evidence that NO is involved in memory, behaviour and emotion.8–10
As evidence supporting the relation between NO and central nervous system function continues to accumulate, evidence of a relation between NO and schizophrenia is also increasing. In 1993, Akbarian et al11,12 reported a distorted distribution of nicotineamide-adenine dinucleotide phosphate-diaphorase (NADPH-d) neurons in various areas of postmortem brains of people who had schizophrenia.11,12 Given that NADPH-d coexists with NOS, their discovery suggests that there may be an NO production abnormality in the brains of patients with schizophrenia. Karson et al13 later showed that the NOS concentration is increased in the cerebellar vermis of postmortem brains of those who had schizophrenia. By means of ex vivo experiments, Das et al14 showed NOS activity to be significantly elevated in the platelets of drug-naive patients with schizophrenia compared with controls, drug-treated patients with schizophrenia and patients with panic disorder, and Herken et al15 reported a remarkable increase in nitrite plus nitrate levels in red blood cells of patients with schizophrenia compared with control subjects. These findings suggest that there is excess NO production in the brains of individuals with schizophrenia. Excess NO is thought to be neurotoxic owing to the formation of peroxinitrite, a very reactive anion with protonation, which is formed from the reaction of NO with superoxide.16,17
Strauss and colleagues18 proposed that positive and negative symptoms in schizophrenia be studied separately, and in 1980, Crow19 suggested that schizophrenia be divided into 2 types — Type I, which is characterized by positive symptoms, and Type II, which is characterized by negative symptoms and constant symptoms. Later, patients with Type II schizophrenia were reported to have decreased intelligence and enlarged cerebral ventricles, suggesting that neuron loss might underlie the pathogenesis of Type II schizophrenia.20,21 Carpenter and colleages22 further classified negative symptoms into 2 types — primary negative symptoms, which are enduring, and secondary negative symptoms, which are more transient and occur secondary to other factors (e.g., adverse effects of neuroleptics, anxiety, suspiciousness, depression and motor retardation). They termed the subtype of schizophrenia that is characterized by primary negative symptoms “deficit syndrome” and established the criteria for its diagnosis.23 Similarly, Keefe et al24,25 attempted to distinguish Kraepelinian from non-Kraepelinian schizophrenia on the basis of symptom outcome and degree of deterioration.
Given these lines of evidence, we hypothesized that excess NO production may lead to neurodegeneration and the formation of enduring negative symptoms in the brains of patients with the deficit form of schizophrenia. To support this working hypothesis, we investigated the levels of nitrate, a marker of in vivo NO production,26 in plasma from patients with deficit and non-deficit forms of schizophrenia and healthy controls.
Methods
This study was carried out in accordance with the latest version of the Declaration of Helsinki, and the design was approved by the Ethics Committee of the Department of Neuropsychiatry, Keio University. Informed consent was obtained from each patient upon provision of a thorough explanation of the procedures.
The subjects consisted of 25 outpatients (14 females) who met the DSM-IV criteria for schizophrenia on their first visit to our clinics and 12 (6 females) healthy volunteers (controls). Each patient was diagnosed using the Japanese version of the Schedule for the Deficit Syndrome27 (SDS) after at least 1 year of follow-up by an attending psychiatrist. Inter-rater and test–retest reliabilities of the differential diagnosis between the deficit and non-deficit forms of schizophrenia in our group were good (kappa = 0.86, and kappa = 0.93, respectively).27 None of the patients had taken antipsychotics for at least 2 weeks before blood collection, but 6 patients had taken 1 or 2 types of benzodiazepine. Patients with conditions possibly affecting their plasma nitrite and nitrate levels, such as drug abuse and certain diseases (blood, neurological, hepatic, cardiovascular or renal), were excluded from this study. Moreover, none of the subjects had any history of these conditions.
Blood was collected between 1000 and 1200 hours. Plasma nitrite and nitrate concentrations were measured using a high-performance liquid chromatography (ENO-20, Eicom, Kyoto, Japan). The lower detection limit in our laboratory was 0.1 mmol/L.
Hepatic and renal functions and cell counts were determined at the time of blood sampling to confirm that these values were within normal limits. There were 2 athletes and 12 smokers among our subjects. In addition to a general analysis of all subject data, we also conducted an analysis excluding data from the patients who took benzodiazepines, the smokers and the athletes. Exclusion of these subjects did not substantially change the overall findings.
Data are expressed as means (and standard error of the mean [SEM]) and were analyzed with 1-way analysis of variance (ANOVA). Post-hoc analysis was performed with Scheffé’s test.
Results
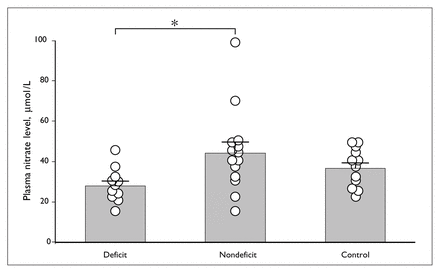
The mean age of deficit patients was 27.8 (SEM 1.4) years, non-deficit patients was 31.9 (SEM 1.5) years and controls was 32.7 (SEM 1.6) years. Mean plasma nitrite levels of deficit patients, non-deficit patients and controls were 4.64 (SEM 0.70) μmol/L, 4.87 (SEM 0.55) μmol/L and 4.61 (SEM 0.83) μmol/L, respectively (F = 0.046, p = 0.95). Mean plasma nitrate levels of deficit patients, non-deficit patients and controls were 28.0 (SEM 2.5) μmol/L, 44.2 (SEM 5.5) μmol/L and 36.8 (SEM 2.8) μmol/L, respectively (Fig. 1). Plasma nitrate levels of deficit patients were significantly lower than those of non-deficit patients (F = 3.87, p = 0.03).
Individual (circles) and mean (and standard error of the mean) (bars) plasma nitrate levels in patients with deficit and non-deficit schizophrenia and controls. Plasma nitrate levels were significantly lower in the deficit than in the non-deficit form (Scheffé’s test, *p < 0.05).
Discussion
It is generally accepted that schizophrenia constitutes a wide spectrum of diseases. Among the many proposals to divide schizophrenia into subgroups,22,24,25 the deficit and non-deficit classification is one of the most heavily investigated. Previous investigations have revealed differences in intelligence, cognitive function, brain structure and brain function between the 2 forms of schizophrenia.28–33 The findings of this study (i.e., different plasma nitrate levels) may further support the heterogeneity between deficit and non-deficit forms of schizophrenia.
Contrary to our working hypothesis, data obtained in this study suggest NO production is diminished in patients with deficit syndrome compared with nondeficit syndrome patients. It remains unclear whether reduced NO production is related to the pathogenesis of deficit syndrome (negative symptoms), but interesting possibilities have been raised in the literature. We previously showed that symptoms of deficit syndrome do not respond to bromperidol, a dopamine D2 receptor antagonist, whereas those of non-deficit syndrome do.34 Amphetamines and related substances, dopamine releaser and dopamine reuptake inhibitors induce only positive symptom-like conditions in animals and humans.35 These findings suggest that factors other than the central dopaminergic system underlie the pathogenesis of deficit syndrome.
On the other hand, the phencyclidine (PCP) model of schizophrenia mimics not only positive symptoms but also negative symptoms,36 suggesting N-methyl-d-asparate (NMDA) receptors may be related to negative symptoms35 (because PCP is a NMDA receptor antagonist). The 3 subtypes of NOS are neuronal (NOS1), inducible (NOS2) and endothelial (NOS3).37 Production of neuronal NO is catalyzed by NOS1, is Ca2+-dependent and is stimulated by activation of NMDA receptors that allow for the influx of Ca2+.38 Moreover, PCP itself was shown to be a suicide inhibitor of NOS in the brain.39 Bird et al40 showed PCP-induced behavioural effects and neuronal activity to be reduced in mice treated with NOS1 antisense oligonucleotides and in NOS1 knockout mice, suggesting the NO system in the brain to be necessary for PCP-induced effects. In addition, nitric oxide donors reportedly block PCP-induced behaviour,41 and inhibitors of NOS have been shown to potentiate PCP-induced behavioural effects and neuronal activity.42 These data suggest that reduction of NMDA receptor-mediated NOS activity might contribute to the pathogenesis of negative symptoms and that the NMDA receptor–NO system might be a target for novel drugs designed to treat the negative symptoms of schizophrenia.
This study is limited in that the source of diminished NO production could not be precisely localized. However, Srivastava et al43 showed reduced nitrite levels in polymorphonuclear leukocytes, in which only NOS1 is constitutively expressed, in patients with schizophrenia. Shinkai et al44 showed the NOS1 gene polymorphism to confer increased susceptibility to schizophrenia. These data suggest that NOS activity in the brain is attenuated in some forms of schizophrenia.
We found no significant difference in plasma nitrite or nitrate levels between patients with schizophrenia in general (deficit plus non-deficit) and controls. This is contrary to previous studies that suggest NO production is increased in brains of individuals with schizophrenia.11–13,15 However, most subjects in previous studies were taking antipsychotics; ours were drug naive. Given the finding that long-term treatment with antipsychotics induces NOS2 mRNA in various regions of the brain, there is a possibility that antipsychotic treatment increased NOS activity in the previous research subjects.45 However, Das et al14 showed increased NOS activity in the platelets of drug-free patients with schizophrenia, and later reported46 decreased plasma nitrate levels of drug-free patients with schizophrenia. Consistent with our results, Srivastava et al43 found no significant change in the plasma total nitrite and nitrate content between drug-free patients and controls. We speculate that the discrepancies reflect the heterogeneous psychotic condition of subjects.
Deficit syndrome is characterized by restricted affect, diminished emotional range, poverty of speech, curbing of interests, diminished sense of purpose and diminished social drive.22,23 Externally, these symptoms are similar to those of depression. However, since we have documented increased plasma nitrate levels in depressed patients compared with those not in a nondepressed state,47 we speculate that the amount of NO production may differ between deficit syndrome and depression.
In conclusion, plasma nitrate levels in patients with deficit-type schizophrenia were significantly lower than those in patients with non-deficit type. These results suggest there is a difference in NO synthesis in patients with deficit and non-deficit types of schizophrenia.
Acknowledgements
We thank Dr. Gohei Yagi and Dr. Masahiro Asai for their introduction of patients and useful discussions.
This study was supported by a Grant-in-Aid for Scientific Research (C) (No. 13671031) from the Japanese Ministry of Education, Culture, Sports, Science and Technology.
Footnotes
Medical subject headings: nitric oxide; nitric-oxide synthase; schizophrenia; signs and symptoms.
Competing interests: None declared for Dr. Nakamura. Dr. Suzuki has received speaker fees from Eisai Pharmaceutical Co. Dr. Nakaki has received speaker fees from Chugai Pharmaceutical Co. Dr. Miyaoka has received speaker fees from Sankyo Pharmaceutical Co., Sumitomo Pharmaceutical Co. and Fujisawa Pharmaceutical Co.
- Received August 28, 2002.
- Revision received December 18, 2002.
- Accepted January 20, 2003.